Similarities and differences between mesenchymal stem/progenitor cells derived from various human tissues
- PMID: 31293717
- PMCID: PMC6600850
- DOI: 10.4252/wjsc.v11.i6.347
Similarities and differences between mesenchymal stem/progenitor cells derived from various human tissues
Abstract
Background: Mesenchymal stromal/stem cells (MSCs) constitute a promising tool in regenerative medicine and can be isolated from different human tissues. However, their biological properties are still not fully characterized. Whereas MSCs from different tissue exhibit many common characteristics, their biological activity and some markers are different and depend on their tissue of origin. Understanding the factors that underlie MSC biology should constitute important points for consideration for researchers interested in clinical MSC application.
Aim: To characterize the biological activity of MSCs during longterm culture isolated from: bone marrow (BM-MSCs), adipose tissue (AT-MSCs), skeletal muscles (SM-MSCs), and skin (SK-MSCs).
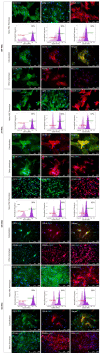
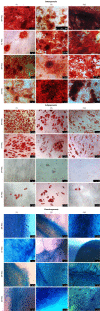
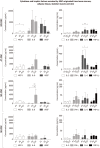
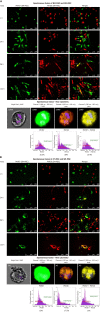
Methods: MSCs were isolated from the tissues, cultured for 10 passages, and assessed for: phenotype with immunofluorescence and flow cytometry, multipotency with differentiation capacity for osteo-, chondro-, and adipogenesis, stemness markers with qPCR for mRNA for Sox2 and Oct4, and genetic stability for p53 and c-Myc; 27 bioactive factors were screened using the multiplex ELISA array, and spontaneous fusion involving a co-culture of SM-MSCs with BM-MSCs or AT-MSCs stained with PKH26 (red) or PKH67 (green) was performed.
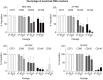
Results: All MSCs showed the basic MSC phenotype; however, their expression decreased during the follow-up period, as confirmed by fluorescence intensity. The examined MSCs express CD146 marker associated with proangiogenic properties; however their expression decreased in AT-MSCs and SM-MSCs, but was maintained in BM-MSCs. In contrast, in SK-MSCs CD146 expression increased in late passages. All MSCs, except BM-MSCs, expressed PW1, a marker associated with differentiation capacity and apoptosis. BM-MSCs and AT-MSCs expressed stemness markers Sox2 and Oct4 in long-term culture. All MSCs showed a stable p53 and c-Myc expression. BM-MSCs and AT-MSCs maintained their differentiation capacity during the follow-up period. In contrast, SK-MSCs and SM-MSCs had a limited ability to differentiate into adipocytes. BM-MSCs and AT-MSCs revealed similarities in phenotype maintenance, capacity for multilineage differentiation, and secretion of bioactive factors. Because AT-MSCs fused with SM-MSCs as effectively as BM-MSCs, AT-MSCs may constitute an alternative source for BM-MSCs.
Conclusion: Long-term culture affects the biological activity of MSCs obtained from various tissues. The source of MSCs and number of passages are important considerations in regenerative medicine.
Keywords: Adipose tissue MSCs; Bone marrow MSCs; Cytokines and trophic factors of MSCs; Mesenchymal stem/progenitor cells; Muscle-derived MSCs; Skin-derived MSCs; Spontaneous fusion of MSCs.
Conflict of interest statement
Conflict-of-interest statement: The authors declare that there is no conflict of interests regarding the publication of this paper.
Figures


Similar articles
-
Differential expression of cell cycle and WNT pathway-related genes accounts for differences in the growth and differentiation potential of Wharton's jelly and bone marrow-derived mesenchymal stem cells.Stem Cell Res Ther. 2017 Apr 26;8(1):102. doi: 10.1186/s13287-017-0555-9. Stem Cell Res Ther. 2017. PMID: 28446235 Free PMC article.
-
Microenvironment in neuroblastoma: isolation and characterization of tumor-derived mesenchymal stromal cells.BMC Cancer. 2018 Nov 27;18(1):1176. doi: 10.1186/s12885-018-5082-2. BMC Cancer. 2018. PMID: 30482160 Free PMC article.
-
Phenotype, donor age and gender affect function of human bone marrow-derived mesenchymal stromal cells.BMC Med. 2013 Jun 11;11:146. doi: 10.1186/1741-7015-11-146. BMC Med. 2013. PMID: 23758701 Free PMC article.
-
The potential of enriched mesenchymal stem cells with neural crest cell phenotypes as a cell source for regenerative dentistry.Jpn Dent Sci Rev. 2017 May;53(2):25-33. doi: 10.1016/j.jdsr.2016.09.001. Epub 2016 Nov 5. Jpn Dent Sci Rev. 2017. PMID: 28479933 Free PMC article. Review.
-
Bone Marrow Microenvironment Involvement in t-MN: Focus on Mesenchymal Stem Cells.Mediterr J Hematol Infect Dis. 2023 Sep 1;15(1):e2023055. doi: 10.4084/MJHID.2023.055. eCollection 2023. Mediterr J Hematol Infect Dis. 2023. PMID: 37705521 Free PMC article. Review.
Cited by
-
Mesenchymal Stem/Stromal Cells and Their Paracrine Activity-Immunomodulation Mechanisms and How to Influence the Therapeutic Potential.Pharmaceutics. 2022 Feb 9;14(2):381. doi: 10.3390/pharmaceutics14020381. Pharmaceutics. 2022. PMID: 35214113 Free PMC article. Review.
-
Challenges and translational considerations of mesenchymal stem/stromal cell therapy for Parkinson's disease.NPJ Regen Med. 2020 Nov 3;5(1):20. doi: 10.1038/s41536-020-00106-y. NPJ Regen Med. 2020. PMID: 33298940 Free PMC article. Review.
-
MSC-EV therapy for bone/cartilage diseases.Bone Rep. 2022 Nov 9;17:101636. doi: 10.1016/j.bonr.2022.101636. eCollection 2022 Dec. Bone Rep. 2022. PMID: 36389627 Free PMC article.
-
Comprehensive comparison of gene expression diversity among a variety of human stem cells.NAR Genom Bioinform. 2022 Nov 29;4(4):lqac087. doi: 10.1093/nargab/lqac087. eCollection 2022 Dec. NAR Genom Bioinform. 2022. PMID: 36458020 Free PMC article.
-
Molecular Imaging of Human Skeletal Myoblasts (huSKM) in Mouse Post-Infarction Myocardium.Int J Mol Sci. 2021 Oct 8;22(19):10885. doi: 10.3390/ijms221910885. Int J Mol Sci. 2021. PMID: 34639225 Free PMC article.
References
-
- Friedenstein AJ, Petrakova KV, Kurolesova AI, Frolova GP. Heterotopic of bone marrow. Analysis of precursor cells for osteogenic and hematopoietic tissues. Transplantation. 1968;6:230–247. - PubMed
-
- Friedenstein A, Kuralesova AI. Osteogenic precursor cells of bone marrow in radiation chimeras. Transplantation. 1971;12:99–108. - PubMed
-
- Caplan AI. Mesenchymal stem cells. J Orthop Res. 1991;9:641–650. - PubMed
-
- Orciani M, Di Primio R. Skin-derived mesenchymal stem cells: isolation, culture, and characterization. Methods Mol Biol. 2013;989:275–283. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

