Driving factors in treatment decision-making of patients seeking medical assistance for infertility: a systematic review
- PMID: 38305635
- PMCID: PMC11063545
- DOI: 10.1093/humupd/dmae001
Driving factors in treatment decision-making of patients seeking medical assistance for infertility: a systematic review
Abstract
Background: ART differs in effectiveness, side-effects, administration, and costs. To improve the decision-making process, we need to understand what factors patients consider to be most important.
Objective and rationale: We conducted this systematic review to assess which aspects of ART treatment (effectiveness, safety, burden, costs, patient-centeredness, and genetic parenthood) are most important in the decision-making of patients with an unfulfilled wish to have a child.
Search methods: We searched studies indexed in Embase, PubMed, PsycINFO, and CINAHL prior to November 2023. Discrete choice experiments (DCEs), surveys, interviews, and conjoint analyses (CAs) about ART were included. Studies were included if they described two or more of the following attributes: effectiveness, safety, burden, costs, patient-centeredness, and genetic parenthood.Participants were men and women with an unfulfilled wish to have a child. From each DCE/CA study, we extracted the beta-coefficients and calculated the relative importance of treatment attributes or, in case of survey studies, extracted results. We assessed the risk of bias using the rating developed by the Grading of Recommendations Assessment, Development and Evaluation working group. Attributes were classified into effectiveness, safety, burden, costs, patient-centeredness, genetic parenthood, and others.
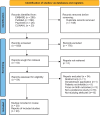
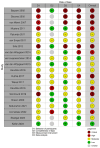
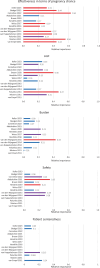
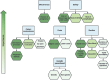
Outcomes: The search identified 938 studies of which 20 were included: 13 DCEs, three survey studies, three interview studies, and one conjoint analysis, with a total of 12 452 patients. Per study, 47-100% of the participants were women. Studies were assessed as having moderate to high risk of bias (critical: six studies, serious: four studies, moderate: nine studies, low: one study). The main limitation was the heterogeneity in the questionnaires and methodology utilized. Studies varied in the number and types of assessed attributes. Patients' treatment decision-making was mostly driven by effectiveness, followed by safety, burden, costs, and patient-centeredness. Effectiveness was rated as the first or second most important factor in 10 of the 12 DCE studies (83%) and the relative importance of effectiveness varied between 17% and 63%, with a median of 34% (moderate certainty of evidence). Of eight studies evaluating safety, five studies valued safety as the first or second most important factor (63%), and the relative importance ranged from 8% to 35% (median 23%) (moderate certainty of evidence). Cost was rated as first or second most important in five of 10 studies, and the importance relative to the other attributes varied between 5% and 47% (median 23%) (moderate certainty of evidence). Burden was rated as first or second by three of 10 studies (30%) and the relative importance varied between 1% and 43% (median 13%) (low certainty of evidence). Patient-centeredness was second most important in one of five studies (20%) and had a relative importance between 7% and 24% (median 14%) (low certainty of evidence). Results suggest that patients are prepared to trade-off some effectiveness for more safety, or less burden and patient-centeredness. When safety was evaluated, the safety of the child was considered more important than the mother's safety. Greater burden (cycle cancellations, number of injections, number of hospital visits, time) was more likely to be accepted by patients if they gained effectiveness, safety, or lower costs. Concerning patient-centeredness, information provision and physician attitude were considered most important, followed by involvement in decision-making, and treatment continuity by the same medical professional. Non-genetic parenthood did not have a clear impact on decision-making.
Wider implications: The findings of this review can be used in future preference studies and can help healthcare professionals in guiding patients' decision-making and enable a more patient-centered approach.
Keywords: ART; acceptability of healthcare; assisted reproduction; child-wish; infertility; patient preference.
© The Author(s) 2024. Published by Oxford University Press on behalf of European Society of Human Reproduction and Embryology.
Conflict of interest statement
The authors have no conflict of interest to declare.
Figures

Similar articles
-
Folic acid supplementation and malaria susceptibility and severity among people taking antifolate antimalarial drugs in endemic areas.Cochrane Database Syst Rev. 2022 Feb 1;2(2022):CD014217. doi: 10.1002/14651858.CD014217. Cochrane Database Syst Rev. 2022. PMID: 36321557 Free PMC article.
-
Economic evaluations of assisted reproductive technologies in high-income countries: a systematic review.Hum Reprod. 2024 May 2;39(5):981-991. doi: 10.1093/humrep/deae039. Hum Reprod. 2024. PMID: 38438132 Free PMC article.
-
Drugs for preventing postoperative nausea and vomiting in adults after general anaesthesia: a network meta-analysis.Cochrane Database Syst Rev. 2020 Oct 19;10(10):CD012859. doi: 10.1002/14651858.CD012859.pub2. Cochrane Database Syst Rev. 2020. PMID: 33075160 Free PMC article.
-
Attributes in stated preference elicitation studies on colorectal cancer screening and their relative importance for decision-making among screenees: a systematic review.Health Econ Rev. 2022 Sep 22;12(1):49. doi: 10.1186/s13561-022-00394-8. Health Econ Rev. 2022. PMID: 36136248 Free PMC article. Review.
-
Interventions for increasing the use of shared decision making by healthcare professionals.Cochrane Database Syst Rev. 2018 Jul 19;7(7):CD006732. doi: 10.1002/14651858.CD006732.pub4. Cochrane Database Syst Rev. 2018. PMID: 30025154 Free PMC article. Review.
Cited by
-
Fertility clinics have a duty of care towards patients who do not have children with treatment.Hum Reprod. 2024 Aug 1;39(8):1591-1598. doi: 10.1093/humrep/deae128. Hum Reprod. 2024. PMID: 38890127 Free PMC article.
References
-
- Abdulrahim B, Scotland G, Bhattacharya S, Maheshwari A.. Assessing couples’ preferences for fresh or frozen embryo transfer: a discrete choice experiment. Hum Reprod 2021;36:2891–2903. - PubMed
-
- Bayram N, van Wely M, van der Veen F, Bossuyt PM, Nieuwkerk P.. Treatment preferences and trade-offs for ovulation induction in clomiphene citrate-resistant patients with polycystic ovary syndrome. Fertil Steril 2005;84:420–425. - PubMed
-
- Behjati Ardakani Z, Navabakhsh M, Ranjbar F, Akhondi MM, Mohseni Tabrizi A.. Step-by-step decision-making process in third party assisted reproduction: a qualitative study. Hum Fertil (Camb) 2022;25:487–498. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

