Antigen Presentation in the Lung
- PMID: 35615351
- PMCID: PMC9124800
- DOI: 10.3389/fimmu.2022.860915
Antigen Presentation in the Lung
Abstract
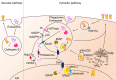
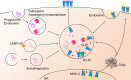
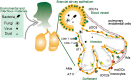
The lungs are constantly exposed to environmental and infectious agents such as dust, viruses, fungi, and bacteria that invade the lungs upon breathing. The lungs are equipped with an immune defense mechanism that involves a wide variety of immunological cells to eliminate these agents. Various types of dendritic cells (DCs) and macrophages (MACs) function as professional antigen-presenting cells (APCs) that engulf pathogens through endocytosis or phagocytosis and degrade proteins derived from them into peptide fragments. During this process, DCs and MACs present the peptides on their major histocompatibility complex class I (MHC-I) or MHC-II protein complex to naïve CD8+ or CD4+ T cells, respectively. In addition to these cells, recent evidence supports that antigen-specific effector and memory T cells are activated by other lung cells such as endothelial cells, epithelial cells, and monocytes through antigen presentation. In this review, we summarize the molecular mechanisms of antigen presentation by APCs in the lungs and their contribution to immune response.
Keywords: antigen cross presentation; antigen presentation; dendritic cells; lung; macrophages.
Copyright © 2022 Kawasaki, Ikegawa and Kawai.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Cross-dressed dendritic cells drive memory CD8+ T-cell activation after viral infection.Nature. 2011 Mar 31;471(7340):629-32. doi: 10.1038/nature09863. Nature. 2011. PMID: 21455179 Free PMC article.
-
Dendritic type, accessory cells within the mammalian thymic microenvironment. Antigen presentation in the dendritic neuro-endocrine-immune cellular network.In Vivo. 1997 Jul-Aug;11(4):351-70. In Vivo. 1997. PMID: 9292303
-
Antigen processing and CD24 expression determine antigen presentation by splenic CD4+ and CD8+ dendritic cells.Immunology. 2008 Mar;123(3):447-55. doi: 10.1111/j.1365-2567.2007.02711.x. Epub 2007 Oct 19. Immunology. 2008. PMID: 17949418 Free PMC article.
-
Antigen presenting cells: Professionals, amateurs, and spectators in the 'long game' of lung immunity.Int J Biochem Cell Biol. 2022 Dec;153:106331. doi: 10.1016/j.biocel.2022.106331. Epub 2022 Nov 8. Int J Biochem Cell Biol. 2022. PMID: 36368596 Review.
-
Salmonella infection of bone marrow-derived macrophages and dendritic cells: influence on antigen presentation and initiating an immune response.FEMS Immunol Med Microbiol. 2000 Apr;27(4):313-20. doi: 10.1111/j.1574-695X.2000.tb01445.x. FEMS Immunol Med Microbiol. 2000. PMID: 10727887 Review.
Cited by
-
Phenotypic and Transcriptional Changes of Pulmonary Immune Responses in Dogs Following Canine Distemper Virus Infection.Int J Mol Sci. 2022 Sep 2;23(17):10019. doi: 10.3390/ijms231710019. Int J Mol Sci. 2022. PMID: 36077417 Free PMC article.
-
Single-cell resolution of human airway epithelial cells exposed to bronchiolitis obliterans-associated chemicals.Am J Physiol Lung Cell Mol Physiol. 2024 Feb 1;326(2):L135-L148. doi: 10.1152/ajplung.00304.2023. Epub 2023 Dec 12. Am J Physiol Lung Cell Mol Physiol. 2024. PMID: 38084407 Free PMC article.
-
Early innate cell interactions with Mycobacterium tuberculosis in protection and pathology of tuberculosis.Front Immunol. 2023 Oct 27;14:1260859. doi: 10.3389/fimmu.2023.1260859. eCollection 2023. Front Immunol. 2023. PMID: 37965344 Free PMC article. Review.
-
Roles of tissue-resident immune cells in immunotherapy of non-small cell lung cancer.Front Immunol. 2023 Dec 7;14:1332814. doi: 10.3389/fimmu.2023.1332814. eCollection 2023. Front Immunol. 2023. PMID: 38130725 Free PMC article. Review.
-
Single-cell combined with transcriptome sequencing to explore the molecular mechanism of cell communication in idiopathic pulmonary fibrosis.J Cell Mol Med. 2024 Jun;28(12):e18499. doi: 10.1111/jcmm.18499. J Cell Mol Med. 2024. PMID: 38887981 Free PMC article.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

