Re-irradiation for malignant glioma: Toward patient selection and defining treatment parameters for salvage
- PMID: 30370358
- PMCID: PMC6200913
- DOI: 10.1016/j.adro.2018.06.005
Re-irradiation for malignant glioma: Toward patient selection and defining treatment parameters for salvage
Abstract
Purpose: Reirradiation for recurrent glioma remains controversial without knowledge of optimal patient selection, dose, fractionation, and normal tissue tolerances. We retrospectively evaluated outcomes and toxicity after conventionally fractionated reirradiation for recurrent high-grade glioma, along with the impact of concurrent chemotherapy.
Methods and materials: We conducted a retrospective review of patients reirradiated for high-grade glioma recurrence between 2007 and 2016 (including patients with initial low-grade glioma). Outcome metrics included overall survival (OS), prognostic factors for survival, and treatment-related toxicity.
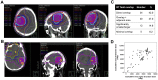
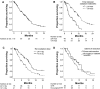
Results: Patients (n = 118; median age 47 years; median Karnofsky performance status score: 80) were re-treated at a median of 28 months (range, 5-214 months) after initial radiation therapy. The median reirradiation dose was 41.4 Gy (range, 12.6-54.0 Gy) to a median lesion volume of 202 cm3 (range, 20-901 cm3). The median cumulative (initial radiation and reirradiation combined) potential maximum brainstem dose was 76.9 Gy (range, 5.0-108.3 Gy) and optic apparatus dose was 56.0 Gy (range, 4.5-90.9 Gy). Of the patients, 56% received concurrent temozolomide, 14%, bevacizumab, and 11%, temozolomide plus bevacizumab; 19% had no chemotherapy. The planned reirradiation was completed by 90% of patients. Median OS from the completion of reirradiation was 9.6 months (95% confidence interval [CI], 7.5-11.7 months) for all patients and 14.0, 11.5, and 6.7 months for patients with initial grade 2, 3, and 4 glioma, respectively. On multivariate analysis, better OS was observed with a >24-month interval between radiation treatments (hazard ratio [HR]: 0.3; 95% CI, 0.2-0.5; P < .001), reirradiation dose >41.4 Gy (HR: 0.6; 95% CI, 0.4-0.9; P = .03), and gross total resection before reirradiation (HR: 0.6, 95% CI, 0.3-0.9; P = .02). Radiation necrosis and grade ≥3 late neurotoxicity were both minimal (<5%). No symptomatic persistent brainstem or optic nerve/chiasm injury was identified.
Conclusions: Salvage reirradiation, even at doses >41.4 Gy in conventional fractionation, along with chemotherapy, was safe and well tolerated with meaningful survival duration. These data provide information that may be useful in implementing safe reirradiation treatments for appropriately selected patients and guiding future studies to define optimal reirradiation doses, maximal safe doses to critical structures, and the role of systemic therapy.
Figures
Similar articles
-
Reirradiation with concurrent bevacizumab for recurrent high-grade gliomas in adult patients.Cancer Radiother. 2018 Feb;22(1):9-16. doi: 10.1016/j.canrad.2017.06.013. Epub 2017 Dec 6. Cancer Radiother. 2018. PMID: 29217134
-
Dosimetric Factors and Toxicity in Highly Conformal Thoracic Reirradiation.Int J Radiat Oncol Biol Phys. 2016 Mar 15;94(4):808-15. doi: 10.1016/j.ijrobp.2015.12.007. Epub 2015 Dec 17. Int J Radiat Oncol Biol Phys. 2016. PMID: 26831903
-
Intensity modulated radiation therapy with pulsed reduced dose rate as a reirradiation strategy for recurrent central nervous system tumors: An institutional series and literature review.Pract Radiat Oncol. 2017 Nov-Dec;7(6):e391-e399. doi: 10.1016/j.prro.2017.04.003. Epub 2017 Apr 12. Pract Radiat Oncol. 2017. PMID: 28666902 Clinical Trial.
-
Chemo-reirradiation in persistent/recurrent head and neck cancers.Jpn J Clin Oncol. 2004 Feb;34(2):61-8. doi: 10.1093/jjco/hyh017. Jpn J Clin Oncol. 2004. PMID: 15067097 Review.
-
Radiation and subsequent reirradiation outcomes in the treatment of diffuse intrinsic pontine glioma and a systematic review of the reirradiation literature.Pract Radiat Oncol. 2017 Mar-Apr;7(2):86-92. doi: 10.1016/j.prro.2016.11.005. Epub 2016 Nov 23. Pract Radiat Oncol. 2017. PMID: 28274399 Review.
Cited by
-
Optimising tumour coverage and organ at risk sparing for hypofractionated re-irradiation in glioblastoma.Phys Imaging Radiat Oncol. 2022 Feb 24;21:84-89. doi: 10.1016/j.phro.2022.02.012. eCollection 2022 Jan. Phys Imaging Radiat Oncol. 2022. PMID: 35243037 Free PMC article.
-
The Patterns of Failure and Prognostic Impact of Tumor Location in Patients Undergoing Reirradiation for Glioblastoma.Cureus. 2024 Sep 6;16(9):e68820. doi: 10.7759/cureus.68820. eCollection 2024 Sep. Cureus. 2024. PMID: 39371788 Free PMC article.
-
Re-irradiation for high-grade gliomas: Has anything changed?World J Clin Oncol. 2021 Sep 24;12(9):767-786. doi: 10.5306/wjco.v12.i9.767. World J Clin Oncol. 2021. PMID: 34631441 Free PMC article. Review.
-
High-dose salvage re-irradiation for recurrent/progressive adult diffuse glioma: healing or hurting?Clin Transl Oncol. 2021 Jul;23(7):1358-1367. doi: 10.1007/s12094-020-02526-0. Epub 2021 Feb 2. Clin Transl Oncol. 2021. PMID: 33528810
-
Re-irradiation for recurrent high-grade glioma: an analysis of prognostic factors for survival and predictors of radiation necrosis.J Neurooncol. 2023 Jul;163(3):541-551. doi: 10.1007/s11060-023-04340-4. Epub 2023 May 31. J Neurooncol. 2023. PMID: 37256526
References
-
- Howard S.P., Krauze A., Chan M.D., Tsien C., Tomé W.A. The evolving role for re-irradiation in the management of recurrent grade 4 glioma. J Neurooncol. 2017;134:523–530. - PubMed
-
- Combs S.E., Bischof M., Welzel T. Radiochemotherapy with temozolomide as re-irradiation using high precision fractionated stereotactic radiotherapy (FSRT) in patients with recurrent gliomas. J Neurooncol. 2008;89:205–210. - PubMed
-
- Combs S.E., Thilmann C., Edler L., Debus J., Schulz-Ertner D. Efficacy of fractionated stereotactic reirradiation in recurrent gliomas: Long-term results in 172 patients treated in a single institution. J Clin Oncol. 2005;23:8863–8869. - PubMed
-
- Flieger M., Ganswindt U., Schwarz S.B. Re-irradiation and bevacizumab in recurrent high-grade glioma: An effective treatment option. J Neurooncol. 2014;117:337–345. - PubMed
LinkOut - more resources
Full Text Sources

