Attenuated allergic airway hyperresponsiveness in C57BL/6 mice is associated with enhanced surfactant protein (SP)-D production following allergic sensitization
- PMID: 14748931
- PMCID: PMC314399
- DOI: 10.1186/1465-9921-4-15
Attenuated allergic airway hyperresponsiveness in C57BL/6 mice is associated with enhanced surfactant protein (SP)-D production following allergic sensitization
Abstract
Background: C57BL/6 mice have attenuated allergic airway hyperresponsiveness (AHR) when compared with Balb/c mice but the underlying mechanisms remain unclear. SP-D, an innate immune molecule with potent immunosuppressive activities may have an important modulatory role in the allergic airway response and the consequent physiological changes. We hypothesized that an elevated SP-D production is associated with the impaired ability of C57BL/6 mice to develop allergic AHR.
Methods: SP-D mRNA and protein expression was investigated during development of allergic airway changes in a model of Aspergillus fumigatus (Af)-induced allergic inflammation. To study whether strain dependency of allergic AHR is associated with different levels of SP-D in the lung, Balb/c and C57BL/6 mice were compared.
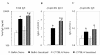
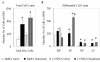
Results: Sensitization and exposure to Af induced significant airway inflammation in both mouse strains in comparison with naïve controls. AHR to acetylcholine however was significantly attenuated in C57BL/6 mice in spite of increased eosinophilia and serum IgE when compared with Balb/c mice (p < 0.05). Af challenge of sensitized C57BL/6 mice induced a markedly increased SP-D protein expression in the SA surfactant fraction (1,894 +/- 170% of naïve controls) that was 1.5 fold greater than the increase in Balb/c mice (1,234 +/- 121% p < 0.01). These changes were selective since levels of the hydrophobic SP-B and SP-C and the hydrophilic SP-A were significantly decreased following sensitization and challenge with Af in both strains. Further, sensitized and exposed C57BL/6 mice had significantly lower IL-4 and IL-5 in the BAL fluid than that of Balb/c mice (p < 0.05).
Conclusions: These results suggest that enhanced SP-D production in the lung of C57BL/6 mice may contribute to an attenuated AHR in response to allergic airway sensitization. SP-D may act by inhibiting synthesis of Th2 cytokines.
Figures



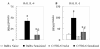
Similar articles
-
Surfactant protein D inhibits early airway response in Aspergillus fumigatus-sensitized mice.Clin Exp Allergy. 2006 Jul;36(7):930-40. doi: 10.1111/j.1365-2222.2006.02524.x. Clin Exp Allergy. 2006. PMID: 16839409
-
Aspergillus fumigatus-induced allergic airway inflammation alters surfactant homeostasis and lung function in BALB/c mice.Am J Respir Cell Mol Biol. 2001 Jul;25(1):45-50. doi: 10.1165/ajrcmb.25.1.4391. Am J Respir Cell Mol Biol. 2001. PMID: 11472974
-
Ozone Inhalation Attenuated the Effects of Budesonide on Aspergillus fumigatus-Induced Airway Inflammation and Hyperreactivity in Mice.Front Immunol. 2019 Sep 13;10:2173. doi: 10.3389/fimmu.2019.02173. eCollection 2019. Front Immunol. 2019. PMID: 31572383 Free PMC article.
-
Protective roles of pulmonary surfactant proteins, SP-A and SP-D, against lung allergy and infection caused by Aspergillus fumigatus.Immunobiology. 2002 Sep;205(4-5):610-8. doi: 10.1078/0171-2985-00158. Immunobiology. 2002. PMID: 12396019 Review.
-
Surfactant proteins SP-A and SP-D as modulators of the allergic inflammation in asthma.Pathobiology. 2002-2003;70(5):287-92. doi: 10.1159/000070744. Pathobiology. 2002. PMID: 12771511 Review.
Cited by
-
Susceptibility to ozone-induced airway inflammation is associated with decreased levels of surfactant protein D.Respir Res. 2006 Jun 1;7(1):85. doi: 10.1186/1465-9921-7-85. Respir Res. 2006. PMID: 16740162 Free PMC article.
-
Lung effector memory and activated CD4+ T cells display enhanced proliferation in surfactant protein A-deficient mice during allergen-mediated inflammation.J Immunol. 2011 Mar 1;186(5):2842-9. doi: 10.4049/jimmunol.0904190. Epub 2011 Jan 21. J Immunol. 2011. PMID: 21257967 Free PMC article.
-
Protective role of the lung collectins surfactant protein A and surfactant protein D in airway inflammation.J Allergy Clin Immunol. 2008 Nov;122(5):861-79; quiz 880-1. doi: 10.1016/j.jaci.2008.10.014. J Allergy Clin Immunol. 2008. PMID: 19000577 Free PMC article.
-
Nitric oxide mediates relative airway hyporesponsiveness to lipopolysaccharide in surfactant protein A-deficient mice.Am J Respir Cell Mol Biol. 2011 Feb;44(2):175-84. doi: 10.1165/rcmb.2009-0284OC. Epub 2010 Mar 26. Am J Respir Cell Mol Biol. 2011. Retraction in: Am J Respir Cell Mol Biol. 2016 Nov;55(5):758. doi: 10.1165/rcmb.555retraction. PMID: 20348208 Free PMC article. Retracted.
-
Group 2 innate lymphoid cells mediate ozone-induced airway inflammation and hyperresponsiveness in mice.J Allergy Clin Immunol. 2016 Feb;137(2):571-8. doi: 10.1016/j.jaci.2015.06.037. Epub 2015 Aug 15. J Allergy Clin Immunol. 2016. PMID: 26282284 Free PMC article.
References
-
- Nicolaides NC, Holroyd KJ, Ewart SL, Eleff SM, Kiser MB, Dragwa CR, Sullivan CD, Grasso L, Zhang LY, Messler CJ, Zhou T, Kleeberger SR, Buetow KH, Levitt RC. Interleukin 9: a candidate gene for asthma. Proc Natl Acad Sci U S A. 1997;94:13175–13180. doi: 10.1073/pnas.94.24.13175. - DOI - PMC - PubMed
-
- Takeda K, Haczku A, Lee JJ, Irvin CG, Gelfand EW. Strain dependence of airway hyperresponsiveness reflects differences in eosinophil localization in the lung. Am J Physiol Lung Cell Mol Physiol. 2001;281:L394–L402. - PubMed
-
- Zhang Y, Lamm WJ, Albert RK, Chi EY, Henderson W.R.,Jr., Lewis DB. Influence of the route of allergen administration and genetic background on the murine allergic pulmonary response. Am J Respir Crit Care Med. 1997;155:661–669. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

