Abstract
Aptamers, composed of single-stranded DNA or RNA oligonucleotides that interact with target molecules through a specific three-dimensional structure, are selected from pools of combinatorial oligonucleotide libraries. With their high specificity and affinity for target proteins, ease of synthesis and modification, and low immunogenicity and toxicity, aptamers are considered to be attractive molecules for development as anticancer therapeutics. Two aptamers - one targeting nucleolin and a second targeting CXCL12 - are currently undergoing clinical trials for treating cancer patients, and many more are under study. In this mini-review, we present the current clinical status of aptamers and aptamer-based cancer therapeutics. We also discuss advantages, limitations, and prospects for aptamers as cancer therapeutics. [BMB Reports 2015; 48(4): 234-237]
Keywords: Application, Aptamer, Cancer, Oligonucleotide, Therapeutics
APTAMERS AS ATTRACTIVE CANDIDATES FOR TARGETED CANCER THERAPIES
While ‘traditional’ cytotoxic chemotherapies usually kill rapidly dividing cells in the body by interfering with cell division, targeted cancer therapies are designed to interfere with specific molecules needed for tumor growth and progression. Given their greater precision and potential for causing fewer side effects, targeted cancer therapies have become a major focus of cancer research. Typically, targeted cancer therapeutics are classified broadly as small chemicals, peptides, nucleic acids, and monoclonal antibodies. Of these, therapies based on monoclonal antibodies, which can bind to target molecules with high specificity and affinity, are among the most successful and important current strategies for treating cancer patients (1). More than 30 therapeutic antibodies have been used clinically, and hundreds more are undergoing clinical trials (2). Although monoclonal antibodies have many advantages, monoclonal antibody-based medications face a number of issues that have prevented their more widespread use. For example, the high cost of therapeutic monoclonal antibody development is beyond the easy reach of many researchers. The extremely high production costs reflect the requirements for very large cultures of mammalian cells and extensive purification steps under Good Manufacturing Practice (GMP) conditions, but they hamper the widespread use of these drugs (3). Another issue is the therapeutic efficacy of monoclonal antibodies: because monoclonal antibodies are large (∼150 kDa), tumor penetration may be limited (3-5), especially in the case of solid tumors, where entry into tumor tissue from blood vessels is critical for drug efficacy (6). As a consequence of these limitations, whereas over 85% of human cancers are solid tumors (7), only eight monoclonal antibodies that have obtained US Food and Drug Administration (FDA) approval for cancer therapy are used routinely with solid tumors.
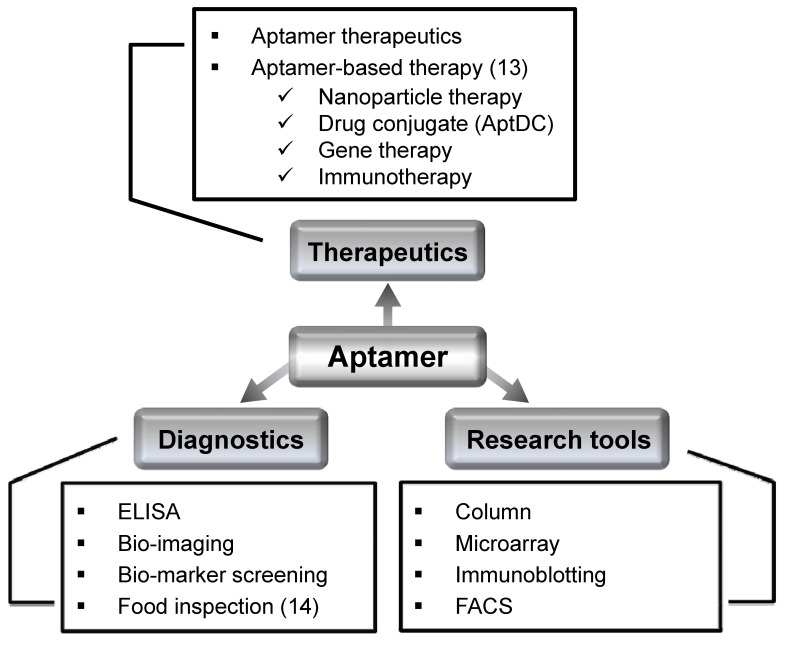
Aptamers, which are composed of short, single-stranded DNA or RNA oligonucleotides, are often compared to antibodies because of their shared high specificity and affinity for target molecules (8, 9). Since the development in 1990 of the ‘SELEX’ (systematic evolution of ligands by exponential enrichment) system-an aptamer screening method-aptamers have come to be regarded as powerful therapeutic, diagnostic, and basic research tools (Fig. 1) (10-12). Over the past two decades, aptamers have attracted increasing attention in the field of cancer therapeutics because they have several important advantages over other targeted therapeutics (Table 1). The fact that aptamers are obtained by chemical synthesis reduces their production costs, compared with monoclonal antibodies. It also means that chemical modifications can be easily and accurately introduced to fulfill different diagnostic and therapeutic purposes (15). Aptamers also show good thermostability and longterm stability as dry powders or in solution (16), and exhibit low immunogenicity and toxicity (17). Notably, aptamers are relatively small, compared with therapeutic monoclonal antibodies, and are thus expected to show greater penetration into tumor tissues (13).
Fig. 1. Possible applications of aptamers. Aptamers bind to target molecules with high affinity and specificity. Because of these and other unique properties, aptamers are ideal tools for broad applications in therapeutics, diagnostics, and basic research.
Table 1. Points to consider for successful cancer therapeutics.
| Properties | Requirements | Candidates |
|---|---|---|
|
| ||
| Target specificity & Binding affinity | Low nM∼pM | Antibodies, Aptamers, Peptides |
| Screening & Production Efforts | Screening: in vitro Fast, Low cost | Peptides, Aptamers |
| Immunogenicity | Low | Humanized antibodies, Aptamers |
| Modification | Easy to conjugation | Small molecules, Peptides, Aptamers |
| Stability | High pharmacokinetics & pharmacodynamics | Antibodies |
APTAMERS IN CLINICAL TRIALS FOR CANCER TARGETS
AS1411. AS1411, a quadruplex-forming guanine-rich (G-rich) 26-mer DNA aptamer, is the most advanced aptamer and the first to enter clinical trials as a cancer therapeutic agent. AS1411 targets the protein nucleolin (18), which plays essential roles in cell growth and death through its involvement in rRNA transport and DNA transcription, replication, and recombination (19). Nucleolin, a nucleus- and cytoplasm-resident protein in normal cells, is overexpressed in the plasma membrane of many types of cancer, including lung cancer, breast cancer, prostate cancer, lymphocytic leukemia, and hepatocellular carcinoma (20). AS1411, developed by Antisoma, inhibits the proliferation of a wide range of cancer cell lines through a mechanism thought to involve disruption of the interaction of nucleolin with its binding partners. The steps involved in AS1411-induced cancer cell death have been proposed to include aptamer internalization via membrane nucleolin, interference with DNA replication, causing S-phase arrest, and stabilization of the mRNA for the anti-apoptotic protein, B-cell lymphoma protein 2 (BCL-2) (18, 20). AS1411, which exhibits minimal toxicity in patients with advanced solid tumors (21), is currently in Phase II clinical trials for acute myeloid leukemia (AML) and metastatic renal cell cancer (20).
NOX-A12. NOX-A12, which is developed by Noxxon Pharma, is a 45-mer long configuration (Spiegelmer) RNA aptamer that is linked to a 40-kDa polyethylene glycol (PEG). NOX-A12 targets CXCL12/SDF-1 (CXC chemokine ligand 12/stromal cell derived factor-1) (22), a chemokine that acts through binding to CXCR4 and CXCR7 chemokine receptors to play diverse roles in cancer biology, including regulation of leukemia stem cell migration to the bone marrow (23) and tumor growth and metastasis. CXCL12/SDF-1 expressed on leukemic cells also responds to the tissue microenvironment to play a role in the pathophysiology of chronic lymphocytic leukemia (CLL) (24). Neutralization of CXCL12/SDF-1 by NOX-A12 also has the potential to interfere with anchoring of leukemia stem cells in the bone marrow, allowing these cells to re-enter the cell cycle and become available for chemotherapeutic attack (25). The unique mirror-image configuration of NOXA12 makes the oligonucleotide resistant to hydrolysis and prevents hybridization with other nucleic acids (26). It has also recently been reported that NOX-A12 effectively inhibits cancer recurrence following irradiation in a glioblastoma multiforme model (27). NOX-A12 is currently in Phase II studies, designed to assess its therapeutic potential against CLL and multiple myeloma (26).
APTAMER-BASED TARGETED CANCER THERAPIES
One of the biggest advantages of aptamers, compared with antibodies, is the ease with which they can be modified chemically while retaining target specificity. Accordingly, there have been numerous efforts to combine the high target-specificity of aptamers with other anticancer modalities to provide targeted delivery of a variety of drug payloads. In these applications, aptamers that target cancer-specific membrane proteins mediate precise delivery of anti-cancer agents, such as nanoparticles, siRNA/miRNA, or cytotoxic drugs, to tumor cells (28). After binding target membrane proteins, aptamers are internalized into the cell together with their drug payload. Ultimately, the drugs are then released from the target molecules and exert their anticancer functions by damaging DNA or inhibiting microtubule polymerization (29). In one example of a nanoparticle designed for prostate cancer therapy, an RNA aptamer targeting prostate-specific membrane antigen (PSMA) was conjugated with a PLA (polylactide)-PEG or PLGA (polylactide-co-glycolide)-PEG nanoparticle encapsulating docetaxel (30, 31). In another example, paclitaxel-containing PLGA conjugated with an aptamer against mucin-1 (MUC1) was used to target MUC1-expressing cancer cells (32). siRNA/miRNA payloads have also been conjugated directly to aptamers. For example, chimeric complexes of Plk1 or Bcl2 siRNA-PSMA aptamers and doxorubicin-PSMA aptamers have been developed for inhibiting PSMA-expressing prostate cancers (33). Aptamerdrug conjugates (ApDCs), which are conceptually similar to antibody-drug conjugates (ADCs), are also promising technologies for targeted cancer therapy because they can enhance therapeutic efficacy while reducing associated toxicities (34). Several potential problems with the ADCs approach remain to be resolved, such as undefined antibody-toxin ratios due to heterogeneous drug conjugation, a tendency to aggregate during synthesis, poor pharmacokinetics, and loss of immune reactivity (35). However, the beneficial properties of aptamers, such as accurate site conjugation and high solubility (> 150 mg/ml) (16), may ultimately surmount these potential issues.
LIMITATIONS OF APTAMERS AS CANCER THERAPEUTICS
When aptamers were first introduced, they garnered considerable attention as cancer therapeutics because of their advantages over monoclonal antibody therapeutics, highlighted above. However, even after 20 years, only two aptamers have reached clinical trials. Before aptamers can achieve widespread clinical application, they must clear several hurdles.
Degradation by nucleases. Because aptamers are composed of DNA or RNA oligonucleotides, they are rapidly degraded by exo- and endonucleases (36): the half-life of unmodified nucleotide aptamers in blood can be as short as 2 min (37). To increase the serum half-life of aptamers, researchers have introduced chemical modifications into the sugar moiety or phosphodiester linkages.“Capping” oligonucleotides by modification of 3’ and/or 5’ends of nucleic acid strands protects aptamers from attacks by exonucleases (36). One commonly used approach that achieves such a protective effect is incorporation of an inverted oligonucleotide at the 3’-terminus. The most widely used method for protecting against degradation by endonucleases is the incorporation of a fluoro or O-methyl group at the 2’position of the sugar moiety (38). Such modifications are typically combined to confer maximal protection. For example, pegaptanib sodium (Macugen), the first aptamer approved by the FDA in 2004, is 3’-capped, 5’-PEGylated, and internally modified with 2’-fluoro-pyrimidines and 2’-O-methyl-purines modifications that collectively extended the aptamer half-life to 131 h (39). Various modified nucleotides, including 2’amino pyrimidines, boranophosphate internucleotide linkages, 5-modified pyrimidines, and/or 4’thio pyrimidines, have also been used to increase the nuclease-resistant properties of aptamers (36).
Renal clearance. Aptamers usually range in size from 5 to 15 kDa (40). Thus, they are susceptible to rapid elimination from the blood by renal filtration. Target accessibility can be enhanced by increasing the size of an aptamer through conjugation to bulky molecules, such as high-molecular-weight PEG polymers, cholesterol, or certain peptides (41). Because the molecular mass cutoff for the renal glomerulus is 3050 kDa (42), 40-kDa PEGylation has been used extensively for extending the circulation half-life of aptamers. The circulation halflife of un-PEGylated aptamers is less than 20 min, but increases to as long as 1 day for 40-kDa PEGylated aptamers (43).
CONCLUSIONS AND PERSPECTIVES
Although aptamers have many properties that make them potentially advantageous for use as cancer therapeutics, their current market prospects are discouraging. Notable in this context is the failure of pegaptanib to make inroads in the marketplace dominated by therapeutic antibodies, such as bevacizumab (Avastin) or ranibizumab (Lucentis) (44, 45). Despite such setbacks, aptamers remain attractive molecules with the opportunity for development as cancer therapeutics. For aptamers to achieve success in the cancer therapeutic market, they will need to take full advantage of their unique features, rather than compete directly with antibody therapeutics. Our expectation is that efficacious aptamer-based anticancer agents will be developed in the near future.
Acknowledgments
This work was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF), funded by the Ministry of Education (NRF-2012R1A1A2004469) and the research grants from the National Cancer Center Grants (NCC1410270).
References
- 1.Scott AM, Wolchok JD, Old LJ. Antibody therapy of cancer. Nat Rev Cancer. (2012);12:278–287. doi: 10.1038/nrc3236. [DOI] [PubMed] [Google Scholar]
- 2.Liu JKH. The history of monoclonal antibody development - Progress, remaining challenges and future innovations. Ann Med Surg. (2014);3:113–116. doi: 10.1016/j.amsu.2014.09.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Chames P, Van Regenmortel M, Weiss E, Baty D. Therapeutic antibodies: successes, limitations and hopes for the future. Br J Pharmacol. (2009);157:220–233. doi: 10.1111/j.1476-5381.2009.00190.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Tabrizi M, Bornstein GG, Suria H. Biodistribution mechanisms of therapeutic monoclonal antibodies in health and disease. AAPS J. (2010);12:33–43. doi: 10.1208/s12248-009-9157-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Miller MJ, Foy KC, Kaumaya PT. Cancer immunotherapy: present status, future perspective, and a new paradigm of peptide immunotherapeutics. Discov Med. (2013);15:166–176. [PubMed] [Google Scholar]
- 6.Jain RK, Stylianopoulos T. Delivering nanomedicine to solid tumors. Nat Rev Clin Oncol. (2010);7:653–664. doi: 10.1038/nrclinonc.2010.139. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Beckman RA, Weiner LM, Davis HM. Antibody constructs in cancer therapy: protein engineering strategies to improve exposure in solid tumors. Cancer. (2007);109:170–179. doi: 10.1002/cncr.22402. [DOI] [PubMed] [Google Scholar]
- 8.Sung HJ, Choi S, Lee JW, et al. Inhibition of human neutrophil activity by an RNA aptamer bound to interleukin-8. Biomaterials. (2014);35:578–589. doi: 10.1016/j.biomaterials.2013.09.107. [DOI] [PubMed] [Google Scholar]
- 9.Kim YH, Sung HJ, Kim S, et al. An RNA aptamer that specifically binds pancreatic adenocarcinoma up-regulated factor inhibits migration and growth of pancreatic cancer cells. Cancer Lett. (2011);313:76–83. doi: 10.1016/j.canlet.2011.08.027. [DOI] [PubMed] [Google Scholar]
- 10.Tuerk C, Gold L. Systematic evolution of ligands by exponential enrichment: RNA ligands to bacteriophage T4 DNA polymerase. Science. (1990);249:505–510. doi: 10.1126/science.2200121. [DOI] [PubMed] [Google Scholar]
- 11.Keefe AD, Pai S, Ellington A. Aptamers as therapeutics. Nat Rev Drug Discov. (2010);9:537–550. doi: 10.1038/nrd3141. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Kong HY, Byun J. Nucleic Acid aptamers: new methods for selection, stabilization, and application in biomedical science. Biomol Ther. (2013);21:423–434. doi: 10.4062/biomolther.2013.085. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Sun H, Zhu X, Lu PY, Rosato RR, Tan W, Zu Y. Oligonucleotide aptamers: new tools for targeted cancer therapy. Mol Ther Nucleic Acids. (2014);3:e182. doi: 10.1038/mtna.2014.32. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Dong Y, Xu Y, Yong W, Chu X, Wang D. Aptamer and its potential applications for food safety. Crit Rev Food Sci Nutr. (2014);54:1548–1561. doi: 10.1080/10408398.2011.642905. [DOI] [PubMed] [Google Scholar]
- 15.Song KM, Lee S, Ban C. Aptamers and Their Biological Applications. Sensors (Basel) (2012);12:612–631. doi: 10.3390/s120100612. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Tan W, Wang H, Chen Y, et al. Molecular aptamers for drug delivery. Trends Biotechnol. (2011);29:634–640. doi: 10.1016/j.tibtech.2011.06.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Pendergrast PS, Marsh HN, Grate D, Healy JM, Stanton M. Nucleic acid aptamers for target validation and therapeutic applications. J Biomol Tech. (2005);16:224–234. [PMC free article] [PubMed] [Google Scholar]
- 18.Bates PJ, Laber DA, Miller DM, Thomas SD, Trent JO. Discovery and development of the G-rich oligonucleotide AS1411 as a novel treatment for cancer. Exp Mol Pathol. (2009);86:151–164. doi: 10.1016/j.yexmp.2009.01.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Tajrishi MM, Tuteja R, Tuteja N. Nucleolin: The most abundant multifunctional phosphoprotein of nucleolus. Commun Integr Biol. (2011);4:267–275. doi: 10.4161/cib.4.3.14884. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Zhu J, Huang H, Dong S, Ge L, Zhang Y. Progress in aptamer-mediated drug delivery vehicles for cancer targeting and its implications in addressing chemotherapeutic challenges. Theranostics. (2014);4:931–944. doi: 10.7150/thno.9663. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Laber DA, Sharma VR, Bhupalam L, Taft B, Hendler FJ, Barnhart KM. Update on the first phase I study of AGRO100 in advanced cancer. J Clin Oncol. (2005);23:3064. [Google Scholar]
- 22.Ni X, Castanares M, Mukherjee A, Lupold SE. Nucleic acid aptamers: clinical applications and promising new horizons. Curr Med Chem. (2011);18:4206–4214. doi: 10.2174/092986711797189600. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Nagasawa T, Hirota S, Tachibana K, et al. Defects of B-cell lymphopoiesis and bone-marrow myelopoiesis in mice lacking the CXC chemokine PBSF/SDF-1. Nature. (1996);382:635–638. doi: 10.1038/382635a0. [DOI] [PubMed] [Google Scholar]
- 24.Sun X, Cheng G, Hao M, et al. CXCL12 / CXCR4 / CXCR7 chemokine axis and cancer progression. Cancer Metastasis Rev. (2010);29:709–722. doi: 10.1007/s10555-010-9256-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Shum KT, Zhou J, Rossi JJ. Nucleic Acid Aptamers as Potential Therapeutic and Diagnostic Agents for Lymphoma. J Cancer Ther. (2013);4:872–890. doi: 10.4236/jct.2013.44099. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Hoellenriegel J, Zboralski D, Maasch C, et al. The Spiegelmer NOX-A12, a novel CXCL12 inhibitor, interferes with chronic lymphocytic leukemia cell motility and causes chemosensitization. Blood. (2014);123:1032–1039. doi: 10.1182/blood-2013-03-493924. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Liu SC, Alomran R, Chernikova SB, et al. Blockade of SDF-1 after irradiation inhibits tumor recurrences of autochthonous brain tumors in rats. Neuro Oncol. (2014);16:21–28. doi: 10.1093/neuonc/not149. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Zhou J, Rossi JJ. Cell-type-specific, Aptamerfunctionalized Agents for Targeted Disease Therapy. Mol Ther Nucleic Acids. (2014);3:e169. doi: 10.1038/mtna.2014.21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Bruno JG. A review of therapeutic aptamer conjugates with emphasis on new approaches. Pharmaceuticals (Basel) (2013);6:340–357. doi: 10.3390/ph6030340. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Farokhzad OC, Jon S, Khademhosseini A, Tran TN, Lavan DA, Langer R. Nanoparticle-aptamer bioconjugates: a new approach for targeting prostate cancer cells. Cancer Res. (2004);64:7668–7672. doi: 10.1158/0008-5472.CAN-04-2550. [DOI] [PubMed] [Google Scholar]
- 31.Farokhzad OC, Cheng J, Teply BA, et al. Targeted nanoparticle-aptamer bioconjugates for cancer chemotherapy in vivo. Proc Natl Acad Sci U S A. (2006);103:6315–6320. doi: 10.1073/pnas.0601755103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Yu C, Hu Y, Duan J, et al. Novel aptamer-nanoparticle bioconjugates enhances delivery of anticancer drug to MUC1-positive cancer cells in vitro. PLoS One. (2011);6:e24077. doi: 10.1371/journal.pone.0024077. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.McNamara JO, Andrechek ER, Wang Y, et al. Cell type-specific delivery of siRNAs with aptamer-siRNA chimeras. Nat Biotechnol. (2006);24:1005–1015. doi: 10.1038/nbt1223. [DOI] [PubMed] [Google Scholar]
- 34.Leal M, Sapra P, Hurvitz SA, et al. Antibody-drug conjugates: an emerging modality for the treatment of cancer. Ann N Y Acad Sci. (2014);1321:41–54. doi: 10.1111/nyas.12499. [DOI] [PubMed] [Google Scholar]
- 35.Perez HL, Cardarelli PM, Deshpande S, et al. Anti-body-drug conjugates: current status and future directions. Drug Discov Today. (2014);19:869–881. doi: 10.1016/j.drudis.2013.11.004. [DOI] [PubMed] [Google Scholar]
- 36.Shigdar S, Macdonald J, O'Connor M, et al. Aptamers as theranostic agents: modifications, serum stability and functionalisation. Sensors (Basel) (2013);13:13624–13637. doi: 10.3390/s131013624. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Griffin LC, Tidmarsh GF, Bock LC, Toole JJ, Leung LL. In vivo anticoagulant properties of a novel nucleotide-based thrombin inhibitor and demonstration of regional anticoagulation in extracorporeal circuits. Blood. (1993);81:3271–3276. [PubMed] [Google Scholar]
- 38.Davydova AS, Vorobjeva MA, Venyaminova AG. Escort aptamers: new tools for the targeted delivery of therapeutics into cells. Acta Naturae. (2011);3:12–29. [PMC free article] [PubMed] [Google Scholar]
- 39.Ng EW, Shima DT, Calias P, Cunningham ET, Jr, Guyer DR, Adamis AP. Pegaptanib, a targeted anti-VEGF aptamer for ocular vascular disease. Nat Rev Drug Discov. (2006);5:123–132. doi: 10.1038/nrd1955. [DOI] [PubMed] [Google Scholar]
- 40.Lakhin AV, Tarantul VZ, Gening LV. Aptamers: problems, solutions and prospects. Acta Naturae. (2013);5:34–43. [PMC free article] [PubMed] [Google Scholar]
- 41.Healy JM, Lewis SD, Kurz M, et al. Pharmacokinetics and biodistribution of novel aptamer compositions. Pharm Res. (2004);21:2234–2246. doi: 10.1007/s11095-004-7676-4. [DOI] [PubMed] [Google Scholar]
- 42.Ruggiero A, Villa CH, Bander E, et al. Paradoxical glomerular filtration of carbon nanotubes. Proc Natl Acad Sci U S A. (2010);107:12369–12374. doi: 10.1073/pnas.0913667107. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Burmeister PE, Lewis SD, Silva RF, et al. Direct in vitro selection of a 2'-O-methyl aptamer to VEGF. Chem Biol. (2005);12:25–33. doi: 10.1016/j.chembiol.2004.10.017. [DOI] [PubMed] [Google Scholar]
- 44.Shapiro A, Lafond A. Anti-VEGF state of the union. Retina Today. (2012);Jan/Feb:32–34. [Google Scholar]
- 45.Kaiser PK, Cruess AF, Bogaert P, Khunti K, Kelly SP. Balancing risk in ophthalmic prescribing: assessing the safety of anti-VEGF therapies and the risks associated with unlicensed medicines. Graefes Arch Clin Exp Ophthalmol. (2012);250:1563–1571. doi: 10.1007/s00417-012-2123-4. [DOI] [PMC free article] [PubMed] [Google Scholar]