Key Points
-
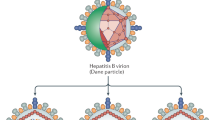
Hepatitis B virus (HBV) and hepatitis C virus (HCV) are both parenterally transmitted enveloped viruses that induce acute and chronic necroinflammatory liver disease. HBV is a partially double-stranded DNA virus and a member of the hepadnaviridae family, whereas HCV is a positive-stranded RNA virus and constitutes a separate genus in the flaviviridae family.
-
HBV and HCV have a narrow host range, which is limited to humans and chimpanzees. Humans are the main natural host for HBV (a single indigenous HBV strain has been identified in chimpanzees in West Africa) and the only natural host for HCV.
-
The most common cause of chronic hepatitis B is vertical transmission from mother to neonate. Vertical transmission is not common for hepatitis C.
-
More than 90% of those individuals who acquire HBV infection as adults, but only 20–40% of those who acquire HCV infection as adults spontaneously recover from all clinical symptoms.
-
Studies of experimentally infected chimpanzees showed that HBV does not induce any detectable changes in the expression of intrahepatic genes in the first weeks of infection. By contrast, HCV upregulates the expression of many intrahepatic genes early after infection.
-
Hepatocytes in which HBV is replicating can be removed by cytotoxic mechanisms or cured by cytokine-mediated, non-cytolytic mechanisms, as shown in transgenic mice (by adoptive transfer of HBV-specific, interferon-γ (IFN-γ)-secreting T cells) and in chimpanzees (by a temporal relationship between HBV clearance and upregulation of intrahepatic IFN-γ expression in the early phase of HBV infection). A reduction in HCV titre at the time of intrahepatic IFN-γ expression has also been shown in HCV infection.
-
Humoral responses in HBV infection are important. HBV core antigen (HBcAg)-specific IgM is an early marker of infection, and the appearance of HBV e antigen (HBeAg)-specific antibodies indicates a reduction in viral titre in chronically infected patients. HBcAg- and HBV surface antigen (HBsAg)-specific IgG persist for life in recovered patients. By contrast, the appearance of HCV-specific antibodies is much more variable: no antibodies develop early after infection, and in some cases, they might not develop at all. HCV-specific antibody titres might decrease to undetectable levels 10–20 years after recovery.
-
Trace amounts of HBV persist after clinical recovery and are controlled by HBV-specific humoral and cellular immune responses. Whether trace amounts of HCV persist long-term after clinical recovery is controversial and requires studies of large patient cohorts.
-
HBV-specific immunity is observed in all clinically recovered patients and is mediated by neutralizing antibodies and T cells. HCV-specific immunity has been described for some, but not all, chimpanzees that recover from an experimental infection, and it is mediated by T cells.
-
HBV- and HCV-specific T-cell responses contribute not only to viral clearance and clinical recovery but also to immune-mediated acute and chronic liver disease.
-
Spontaneous viral clearance, generation of HBsAg-specific-antibody and resolution of disease occurs in ∼2% of patients with chronic hepatitis B each year, and it is temporally correlated with the appearance of HBV-specific T cells in the blood. By contrast, there is no spontaneous viral clearance in patients with chronic hepatitis C.
Abstract
More than 500 million people worldwide are persistently infected with the hepatitis B virus (HBV) and/or hepatitis C virus (HCV) and are at risk of developing chronic liver disease, cirrhosis and hepatocellular carcinoma. Despite many common features in the pathogenesis of HBV- and HCV-related liver disease, these viruses markedly differ in their virological properties and in their immune escape and survival strategies. This review assesses recent advances in our understanding of viral hepatitis, contrasts mechanisms of virus–host interaction in acute hepatitis B and hepatitis C, and outlines areas for future studies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Fattovich, G. Natural history and prognosis of hepatitis B. Semin. Liver Dis. 23, 47–58 (2003).
Seeff, L. B. Natural history of chronic hepatitis C. Hepatology 36, S35–S36 (2002).
Candotti, D., Temple, J., Sarkodie, F. & Allain, J. P. Frequent recovery and broad genotype 2 diversity characterize hepatitis C virus infection in Ghana, West Africa. J. Virol. 77, 7914–7923 (2003).
Guidotti, L. G. et al. Viral clearance without destruction of infected cells during acute HBV infection. Science 284, 825–829 (1999). This study shows that non-cytolytic, cytokine-mediated clearance of HBV from infected hepatocytes occurs during acute HBV infection of non-human primates.
Thimme, R. et al. CD8+ T cells mediate viral clearance and disease pathogenesis during acute hepatitis B virus infection. J. Virol. 77, 68–76 (2003).
Kolykhalov, A. et al. Transmission of hepatitis C by intrahepatic inoculation with transcribed RNA. Science 277, 570–574 (1997).
Yanagi, M., Purcell, R. H., Emerson, S. U. & Bukh, J. Transcripts from a single full-length cDNA clone of hepatitis C virus are infectious when directly transfected into the liver of a chimpanzee. Proc. Natl Acad. Sci. USA 94, 8738–8743 (1997).
Bassett, S. E., Brasky, K. M. & Lanford, R. E. Analysis of hepatitis C virus-inoculated chimpanzees reveals unexpected clinical profiles. J. Virol. 72, 2589–2599 (1998).
Nascimbeni, M. et al. Kinetics of CD4+ and CD8+ memory T cell responses during hepatitis C virus rechallenge of previously recovered chimpanzees. J. Virol. 77, 4781–4793 (2003).
Bigger, C. B., Brasky, K. M. & Lanford, R. E. DNA microarray analysis of chimpanzee liver during acute resolving hepatitis C virus infection. J. Virol. 75, 7059–7066 (2001).
Lanford, R. E. et al. Cross-genotype immunity to hepatitis C virus. J. Virol. 78, 1575–1581 (2004).
Shoukry, N. et al. Memory CD8+ T cells are required for protection from persistent hepatitis C virus infection. J. Exp. Med. 197, 1645–1655 (2003). This paper highlights the importance of memory CD8+ T cells in the control of HCV infection. In vivo depletion of this T-cell subset from chimpanzees that have previously recovered from HCV abrogates protective immunity on rechallenge with HCV.
Grakoui, A. et al. HCV persistence and immune evasion in the absence of memory T cell help. Science 302, 659–662 (2003). An important study showing that in vivo depletion of CD4+ T cells from chimpanzees that have previously recovered from HCV abrogates protective immunity and results in persistent HCV infection on rechallenge.
Logvinoff, C. et al. Neutralizing antibody response during acute and chronic hepatitis C virus infection. Proc. Natl Acad. Sci. USA 101, 10149–10154 (2004). In this study, infectious retroviral pseudotypes that express HCV envelope glycoproteins were used to screen sera for the presence of neutralizing antibodies. The titre of pseudotype-neutralizing antibodies increase late during the course of chronic hepatitis C.
Thimme, R. et al. Viral and immunological determinants of hepatitis C virus clearance, persistence, and disease. Proc. Natl Acad. Sci. USA 99, 15661–15668 (2002).
Ganem, D. & Schneider, R. J. in Fields Virology Vol. 2 (eds Knipe, D. et al.) 2923–2969 (Lippincott Williams & Wilkins, Philadelphia, 2001).
Guidotti, L. G., Matzke, B., Schaller, H. & Chisari, F. V. High-level hepatitis B virus replication in transgenic mice. J. Virol. 69, 6158–6169 (1995).
Bukh, J., Apgar, C. L. & Yanagi, M. Toward a surrogate model for hepatitis C virus: an infectious molecular clone of the GB virus-B hepatitis agent. Virology 262, 470–478 (1999).
Lohmann, V. et al. Replication of subgenomic hepatitis C virus RNAs in a hepatoma cell line. Science 285, 110–113 (1999). The first report to show a subgenomic HCV replicon in a human hepatoma cell line.
Blight, K. J., Kolykhalov, A. A. & Rice, C. M. Efficient initiation of HCV RNA replication in cell culture. Science 290, 1972–1974 (2000). This studies identifies multiple adaptive mutations that confer increased replicative ability to subgenomic HCV replicons in vitro.
Bartosch, B., Dubuisson, J. & Cosset, F. L. Infectious hepatitis C virus pseudo-particles containing functional E1–E2 envelope protein complexes. J. Exp. Med. 197, 633–642 (2003).
McKeating, J. A. et al. Diverse hepatitis C virus glycoproteins mediate viral infection in a CD81-dependent manner. J. Virol. 78, 8496–8505 (2004).
Heller, T. et al. An in vitro model of hepatitis C virion production. Proc. Natl Acad. Sci. USA 102, 2579–2583 (2005).
Lindenbach, B. D. & Rice, C. M. in Fields Virology Vol. 1 (eds Knipe, D. et al.) 991–1041 (Lippincott Williams & Wilkins, Philadelphia, 2001).
Egger, D. et al. Expression of hepatitis C virus proteins induces distinct membrane alterations including a candidate viral replication complex. J. Virol. 76, 5974–5984 (2002).
Thimme, R. et al. Determinants of viral clearance and persistence during acute hepatitis C virus infection. J. Exp. Med. 194, 1395–1406 (2001).
Major, M. E. et al. Hepatitis C virus kinetics and host responses associated with disease and outcome of infection in chimpanzees. Hepatology 39, 1709–1720 (2004).
Gerlach, J. T. et al. Recurrence of hepatitis C virus after loss of virus-specific CD4+ T-cell response in acute hepatitis C. Gastroenterology 117, 933–941 (1999).
Pham, T. N. et al. Hepatitis C virus persistence after spontaneous or treatment-induced resolution of hepatitis C. J. Virol. 78, 5867–5874 (2004).
Takaki, A. et al. Cellular immune responses persist, humoral responses decrease two decades after recovery from a single source outbreak of hepatitis C. Nature Med. 6, 578–582 (2000). This study shows that HCV-specific antibodies decrease to undetectable levels 10–20 years after spontaneous clinical recovery from a single-source outbreak of HCV, whereas HCV-specific T-cell responses are maintained.
Seeff, L. B. et al. Long-term mortality and morbidity of transfusion-associated non-A, non-B, and type C hepatitis: a National Heart, Lung, and Blood Institute collaborative study. Hepatology 33, 455–463 (2001).
Wieland, S., Thimme, R., Purcell, R. H. & Chisari, F. V. Genomic analysis of the host response to hepatitis B virus infection. Proc. Natl Acad. Sci. USA 101, 6669–6674 (2004).
Su, A. I. et al. Genomic analysis of the host response to hepatitis C virus infection. Proc. Natl Acad. Sci. USA 99, 15669–15674 (2002).
McClary, H., Koch, R., Chisari, F. V. & Guidotti, L. G. Relative sensitivity of hepatitis B virus and other hepatotropic viruses to the antiviral effects of cytokines. J. Virol. 74, 2255–2264 (2000).
Wieland, S. F., Guidotti, L. G. & Chisari, F. V. Intrahepatic induction of α/β interferon eliminates viral RNA-containing capsids in hepatitis B virus transgenic mice. J. Virol. 74, 4165–4173 (2000).
Guidotti, L. G. et al. Interferon-regulated pathways that control hepatitis B virus replication in transgenic mice. J. Virol. 76, 2617–2621 (2002).
Robek, M. D., Wieland, S. F. & Chisari, F. V. Inhibition of hepatitis B virus replication by interferon requires proteasome activity. J. Virol. 76, 3570–3574 (2002).
Kakimi, K., Lane, T. E., Chisari, F. V. & Guidotti, L. G. Inhibition of hepatitis B virus replication by activated NK T cells does not require inflammatory cell recruitment to the liver. J. Immunol. 167, 6701–6705 (2001).
Baron, J. L. et al. Activation of a nonclassical NKT cell subset in a transgenic mouse model of hepatitis B virus infection. Immunity 16, 583–594 (2002).
Guidotti, L. G. et al. Intracellular inactivation of the hepatitis B virus by cytotoxic T lymphocytes. Immunity 4, 25–36 (1996).
Fitzgerald, K. A. et al. IKKε and TBK1 are essential components of the IRF3 signaling pathway. Nature Immunol. 4, 491–496 (2003).
Yoneyama, M. et al. The RNA helicase RIG-I has an essential function in double-stranded RNA-induced innate antiviral responses. Nature Immunol. 5, 730–737 (2004).
Balachandran, S., Thomas, E. & Barber, G. N. A FADD-dependent innate immune mechanism in mammalian cells. Nature 432, 401–405 (2004).
Frese, M., Pietschmann, T., Moradpour, D., Haller, O. & Bartenschlager, R. Interferon-α inhibits hepatitis C virus subgenomic RNA replication by an MxA-independent pathway. J. Gen. Virol. 82, 723–733 (2001).
Foy, E. et al. Regulation of interferon regulatory factor-3 by the hepatitis C virus serine protease. Science 300, 1145–1148 (2003).
Taylor, D. R., Shi, S. T., Romano, P. R., Barber, G. N. & Lai, M. M. Inhibition of the interferon-inducible protein kinase PKR by HCV E2 protein. Science 285, 107–110 (1999).
Gale, M. J. Jr et al. Evidence that hepatitis C virus resistance to interferon is mediated through repression of the PKR protein kinase by the nonstructural 5A protein. Virology 230, 217–227 (1997).
Taylor, D. R., Shi, S. T. & Lai, M. M. Hepatitis C virus and interferon resistance. Microbes Infect. 2, 1743–1756 (2000).
Khakoo, S. I. et al. HLA and NK cell inhibitory receptor genes in resolving hepatitis C virus infection. Science 305, 872–874 (2004).
Crotta, S. et al. Inhibition of natural killer cells through engagement of CD81 by the major hepatitis C virus envelope protein. J. Exp. Med. 195, 35–42 (2002).
Tseng, C. T. & Klimpel, G. R. Binding of the hepatitis C virus envelope protein E2 to CD81 inhibits natural killer cell functions. J. Exp. Med. 195, 43–49 (2002).
Jinushi, M. et al. Negative regulation of NK cell activities by inhibitory receptor CD94/NKG2A leads to altered NK cell-induced modulation of dendritic cell functions in chronic hepatitis C virus infection. J. Immunol. 173, 6072–6081 (2004).
Ferrari, C. et al. Cellular immune response to hepatitis B virus-encoded antigens in acute and chronic hepatitis B virus infection. J. Immunol. 145, 3442–3449 (1990).
Rehermann, B. et al. The cytotoxic T lymphocyte response to multiple hepatitis B virus polymerase epitopes during and after acute viral hepatitis. J. Exp. Med. 181, 1047–1058 (1995).
Wedemeyer, H. et al. Impaired effector function of hepatitis C virus-specific CD8+ T cells in chronic hepatitis C virus infection. J. Immunol. 169, 3447–3458 (2002).
Diepolder, H. M. et al. Possible mechanism involving T lymphocyte response to non-structural protein 3 in viral clearance in acute hepatitis C virus infection. Lancet 346, 1006–1007 (1995). The first study to show that vigorous HCV-specific T-cell responses are associated with recovery from acute hepatitis C.
Lechner, F. et al. Analysis of successful immune responses in persons infected with hepatitis C virus. J. Exp. Med. 191, 1499–1512 (2000).
Crispe, I. N. Hepatic T cells and liver tolerance. Nature Rev. Immunol. 3, 51–62 (2003).
Guidotti, L. G. et al. Viral cross talk: intracellular inactivation of the hepatitis B virus during an unrelated viral infection of the liver. Proc. Natl Acad. Sci. USA 93, 4589–4594 (1996).
Pasquetto, V., Guidotti, L. G., Kakimi, K., Tsuji, M. & Chisari, F. V. Host–virus interactions during malaria infection in hepatitis B virus transgenic mice. J. Exp. Med. 192, 529–536 (2000).
Kakimi, K., Guidotti, L. G., Koezuka, Y. & Chisari, F. V. Natural killer T cell activation inhibits hepatitis B virus replication in vivo. J. Exp. Med. 192, 921–930 (2000).
Tsui, L. V., Guidotti, L. G., Ishikawa, T. & Chisari, F. V. Post-transcriptional clearance of hepatitis B virus RNA by cytotoxic T lymphocyte activated hepatocytes. Proc. Natl Acad. Sci. USA 92, 12398–12402 (1995).
Heise, T., Guidotti, L. G. & Chisari, F. V. Characterization of nuclear RNases that cleave hepatitis B virus RNA near the La protein binding site. J. Virol. 75, 6874–6883 (2001).
Guidotti, L. G., McClary, H., Loudis, J. M. & Chisari, F. V. Nitric oxide inhibits hepatitis B virus replication in the livers of transgenic mice. J. Exp. Med. 191, 1247–1252 (2000).
Gerlach, J. T. et al. Acute hepatitis C: high rate of both spontaneous and treatment-induced viral clearance. Gastroenterology 125, 80–88 (2003).
Cooper, S. et al. Analysis of a successful immune response against hepatitis C virus. Immunity 10, 439–449 (1999).
Cheney, I. W. et al. Comparative analysis of anti-hepatitis C virus activity and gene expression mediated by α, β, and γ interferons. J. Virol. 76, 11148–11154 (2002).
Urbani, S. et al. Virus-specific CD8+ lymphocytes share the same effector-memory phenotype but exhibit functional differences in acute hepatitis B and C. J. Virol. 76, 12423–12434 (2002).
Chen, M. et al. Limited humoral immunity in hepatitis C virus infection. Gastroenterology 116, 135–143 (1999).
Maruyama, T. et al. The serology of chronic hepatitis B infection revisited. J. Clin. Invest. 91, 2586–2595 (1993).
Farci, P. et al. Prevention of hepatitis C virus infection in chimpanzees after antibody-mediated in vitro neutralization. Proc. Natl Acad. Sci. USA 91, 7792–7796 (1994). The first study to show neutralization of in vivo infectivity of HCV by specific antibodies.
Forns, X. et al. Vaccination of chimpanzees with plasmid DNA encoding the hepatitis C virus (HCV) envelope E2 protein modified the infection after challenge with homologous monoclonal HCV. Hepatology 32, 618–625 (2000).
Baumert, T. F. et al. Antibodies against hepatitis C virus-like particles and viral clearance in acute and chronic hepatitis C. Hepatology 32, 610–617 (2000).
Hsu, M. et al. Hepatitis C virus glycoproteins mediate pH-dependent cell entry of pseudotyped retroviral particles. Proc. Natl Acad. Sci. USA 100, 7271–7276 (2003).
Yu, M. Y. et al. Neutralizing antibodies to hepatitis C virus (HCV) in immune globulins derived from anti-HCV-positive plasma. Proc. Natl Acad. Sci. USA 101, 7705–7710 (2004).
Farci, P. et al. The outcome of acute hepatitis C predicted by the evolution of the viral quasispecies. Science 288, 339–344 (2000).
Pileri, P. et al. Binding of hepatitis C virus to CD81. Science 282, 938–941 (1998).
Cormier, E. G. et al. CD81 is an entry coreceptor for hepatitis C virus. Proc. Natl Acad. Sci. USA 101, 7270–7274 (2004).
Kawatani, T. et al. Incidence of hepatitis virus infection and severe liver dysfunction in patients receiving chemotherapy for hematologic malignancies. Eur. J. Haematol. 67, 45–50 (2001).
Chazouilleres, O. et al. 'Occult' hepatitis B virus as source of infection in liver transplant recipients. Lancet 343, 142–146 (1994).
Rehermann, B., Ferrari, C., Pasquinelli, C. & Chisari, F. V. The hepatitis B virus persists for decades after patients' recovery from acute viral hepatitis despite active maintenance of a cytotoxic T-lymphocyte response. Nature Med. 2, 1104–1108 (1996). This study shows that HBV-specific cytotoxic CD8+ T cells, as well as trace amounts of HBV DNA, co-exist for decades in patients who have clinically recovered from hepatitis B.
Mizukoshi, E. et al. Cellular immune responses to the hepatitis B virus polymerase. J. Immunol. 173, 5863–5871 (2004).
Rahman, F. et al. Cellular and humoral immune responses induced by intradermal or intramuscular vaccination with the major hepatitis B surface antigen. Hepatology 31, 521–527 (2000).
Hollinger, F. B. et al. Non-A, non-B hepatitis transmission in chimpanzees: a project of the transfusion-transmitted viruses study group. Intervirology 10, 60–68 (1978).
Lai, M. E. et al. Hepatitis C virus in multiple episodes of acute hepatitis in polytransfused thalassaemic children. Lancet 343, 388–390 (1994).
Farci, P. et al. Lack of protective immunity against reinfection with hepatitis C virus. Science 258, 135–140 (1992).
Mehta, S. H. et al. Protection against persistence of hepatitis C. Lancet 359, 1478–1483 (2002).
Chen, M. T. et al. A function of the hepatitis B virus precore protein is to regulate the immune response to the core antigen. Proc. Natl Acad. Sci. USA 101, 14913–14918 (2004).
Whalley, S. A. et al. Evolution of hepatitis B virus during primary infection in humans: transient generation of cytotoxic T-cell mutants. Gastroenterology 127, 1131–1138 (2004).
Rehermann, B., Pasquinelli, C., Mosier, S. M. & Chisari, F. V. Hepatitis B virus (HBV) sequence variation of cytotoxic T lymphocyte epitopes is not common in patients with chronic HBV infection. J. Clin. Invest. 96, 1527–1534 (1995).
Bertoletti, A. et al. Natural variants of cytotoxic epitopes are T-cell receptor antagonists for antiviral cytotoxic T cells. Nature 369, 407–410 (1994).
Shimizu, Y. K. et al. Neutralizing antibodies against hepatitis C virus and the emergence of neutraliziation escape mutant viruses. J. Virol. 68, 1494–1500 (1994).
Erickson, A. L. et al. The outcome of hepatitis C virus infection is predicted by escape mutations in epitopes targeted by cytotoxic T lymphocytes. Immunity 15, 883–895 (2001).
Chang, K. M. et al. Immunological significance of cytotoxic T lymphocyte epitope variants in patients chronically infected by the hepatitis C virus. J. Clin. Invest. 100, 2376–2385 (1997).
Tsai, S. L. et al. Hepatitis C virus variants circumventing cytotoxic T lymphocyte activity as a mechanism of chronicity. Gastroenterology 115, 954–965 (1998).
Frasca, L. et al. Hypervariable region 1 variants act as TCR antagonists for hepatitis C virus-specific CD4+ T cells. J. Immunol. 163, 650–658 (1999).
Seifert, U. et al. Hepatitis C virus mutation affects proteasomal epitope processing. J. Clin. Invest. 114, 250–259 (2004).
Timm, J. et al. CD8 epitope escape and reversion in acute HCV infection. J. Exp. Med. 200, 1593–1604 (2004).
Eisen-Vandervelde, A. L. et al. Hepatitis C virus core selectively suppresses interleukin-12 synthesis in human macrophages by interfering with AP-1 activation. J. Biol. Chem. 279, 43479–43486 (2004).
Kittlesen, D. J., Chianese-Bullock, K. A., Yao, Z. Q., Braciale, T. J. & Hahn, Y. S. Interaction between complement receptor gC1qR and hepatitis C virus core protein inhibits T-lymphocyte proliferation. J. Clin. Invest. 106, 1239–1249 (2000). The first study to show that HCV core protein binds the globular domain of the complement receptor C1q at the surface of T cells and thereby inhibits IL-2 production and T-cell proliferation.
Large, M. K., Kittlesen, D. J. & Hahn, Y. S. Suppression of host immune response by the core protein of hepatitis C virus: possible implications for hepatitis C virus persistence. J. Immunol. 162, 931–938 (1999).
Francavilla, V. et al. Subversion of effector CD8+ T cell differentiation in acute hepatitis C virus infection: exploring the immunological mechanisms. Eur. J. Immunol. 34, 427–437 (2004).
Appay, V. et al. Memory CD8+ T cells vary in differentiation phenotype in different persistent virus infections. Nature Med. 8, 379–385 (2002).
Kanto, T. et al. Impaired allostimulatory capacity of peripheral blood dendritic cells recovered from hepatitis C virus-infected individuals. J. Immunol. 162, 5584–5591 (1999).
Bain, C. et al. Impaired allostimulatory function of dendritic cells in chronic hepatitis C infection. Gastroenterology 120, 512–524 (2001).
Auffermann-Gretzinger, S., Keeffe, E. B. & Levy, S. Impaired dendritic cell maturation in patients with chronic, but not resolved, hepatitis C virus infection. Blood 97, 3171–3176 (2001).
Dolganiuc, A. et al. Hepatitis C virus core and nonstructural protein 3 proteins induce pro- and anti-inflammatory cytokines and inhibit dendritic cell differentiation. J. Immunol. 170, 5615–5624 (2003).
Longman, R. S., Talal, A. H., Jacobson, I. M., Albert, M. L. & Rice, C. M. Presence of functional dendritic cells in patients chronically infected with hepatitis C virus. Blood 103, 1026–1029 (2004).
Rollier, C. et al. Chronic hepatitis C virus infection established and maintained in chimpanzees independent of dendritic cell impairment. Hepatology 38, 851–858 (2003).
Hellier, S. et al. Association of genetic variants of the chemokine receptor CCR5 and its ligands, RANTES and MCP-2, with outcome of HCV infection. Hepatology 38, 1468–1476 (2003).
Accapezzato, D. et al. Hepatic expansion of a virus-specific regulatory CD8+ T cell population in chronic hepatitis C virus infection. J. Clin. Invest. 113, 963–972 (2004).
Sugimoto, K. et al. Suppression of HCV-specific T cells without differential hierarchy demonstrated ex vivo in persistent HCV infection. Hepatology 38, 1437–1448 (2003).
Cabrera, R. et al. An immunomodulatory role for CD4+CD25+ regulatory T lymphocytes in hepatitis C virus infection. Hepatology 40, 1062–1071 (2004).
Boni, C. et al. Antiviral CD8-mediated responses in chronic HCV carriers with HBV superinfection. Hepatology 40, 289–299 (2004).
Rossol, S. et al. Interleukin-12 induction of TH1 cytokines is important for viral clearance in chronic hepatitis B. J. Clin. Invest. 99, 3025–3033 (1997).
Tsai, S. L. et al. Acute exacerbations of chronic type B hepatitis are accompanied by increased T cell responses to hepatitis B core and e antigens. J. Clin. Invest. 89, 87–96 (1992).
Boni, C. et al. Lamivudine treatment can restore T cell responsiveness in chronic hepatitis B. J. Clin. Invest. 102, 968–975 (1998).
Boni, C. et al. Lamivudine treatment can overcome cytotoxic T-cell hyporesponsiveness in chronic hepatitis B: new perspectives for immune therapy. Hepatology 33, 963–971 (2001).
Boni, C. et al. Transient restoration of anti-viral T cell responses induced by lamivudine therapy in chronic hepatitis B. J. Hepatol. 39, 595–605 (2003).
Maini, M. K. et al. The role of virus-specific CD8+ cells in liver damage and viral control during persistent hepatitis B virus (HBV) infection. J. Exp. Med. 191, 1269–1280 (2000).
Ando, K. et al. Mechanisms of class I restricted immunopathology. A transgenic mouse model of fulminant hepatitis. J. Exp. Med. 178, 1541–1554 (1993).
Kakimi, K. et al. Blocking chemokine responsive to γ-2/interferon (IFN)-γ inducible protein and monokine induced by IFN-γ activity in vivo reduces the pathogenetic but not the antiviral potential of hepatitis B virus-specific cytotoxic T lymphocytes. J. Exp. Med. 194, 1755–1766 (2001).
Sitia, G. et al. MMPs are required for recruitment of antigen-nonspecific mononuclear cells into the liver by CTLs. J. Clin. Invest. 113, 1158–1167 (2004).
Liang, T. J. & Heller, T. Pathogenesis of hepatitis C-associated hepatocellular carcinoma. Gastroenterology 127, S62–S71 (2004).
Dammacco, F. et al. The lymphoid system in hepatitis C virus infection: autoimmunity, mixed cryoglobulinemia, and overt B-cell malignancy. Semin. Liver Dis. 20, 143–157 (2000).
Zignego, A. L. & Brechot, C. Extrahepatic manifestations of HCV infection: facts and controversies. J. Hepatol. 31, 369–376 (1999).
Sung, V. M. et al. Establishment of B-cell lymphoma cell lines persistently infected with hepatitis C virus in vivo and in vitro: the apoptotic effects of virus infection. J. Virol. 77, 2134–2146 (2003).
Machida, K. et al. Hepatitis C virus induces a mutator phenotype: enhanced mutations of immunoglobulin and protooncogenes. Proc. Natl Acad. Sci. USA 101, 4262–4267 (2004).
Day, C. L. et al. Ex vivo analysis of human memory CD4 T cells specific for hepatitis C virus using MHC class II tetramers. J. Clin. Invest. 112, 831–842 (2003).
Milich, D. R. & McLachlan, A. The nucleocapsid of hepatitis B virus is both a T-cell-independent and a T-cell-dependent antigen. Science 234, 1398–1401 ( 1986).
Racanelli, V. & Rehermann, B. Hepatitis C virus infection: when silence is deception. Trends Immunol. 24, 456–464 (2003).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Related links
Related links
DATABASES
Infectious Disease Information
FURTHER INFORMATION
Glossary
- NECROINFLAMMATORY
-
A state in which there is morphological evidence of infiltration of inflammatory cells and necrosis of parenchymal cells.
- PROTECTIVE IMMUNITY
-
The immune responses of individuals who have recovered from a primary infection and, on re-exposure to the pathogen, are protected from developing severe disease and chronic infection. Protective immunity can be sterilizing if it protects from a productive infection.
- PSEUDOTYPE PARTICLE
-
A viral particle containing the genome of one virus in the envelope of another virus.
- HEPADNAVIRIDAE
-
A family of hepatotropic DNA viruses, which contain double-stranded DNA genomes and causes hepatitis in humans and animals. Hepadnaviruses have very small genomes of relaxed circular, partially double-stranded DNA. They replicate through an RNA intermediate, which they translate back into DNA using reverse transcriptase. Hepadnaviruses include hepatitis B virus, duck hepatitis virus, heron hepatitis B virus, ground squirrel hepatitis virus and woodchuck hepatitis virus.
- FLAVIVIRIDAE
-
A family of related positive-strand RNA viruses, which consists of three genera: flaviviruses, pestiviruses and hepaciviruses. Flaviviridae replicate by synthesis of a minus-strand RNA intermediate. Dengue virus, bovine viral diarrhoea virus and hepatitis C virus are examples from the three genera.
- NUCLEOCAPSID
-
A nucleic acid and its surrounding protein coat (or capsid). The nucleocapsid forms the basic structural unit of the virion. Depending on the virus, the nucleocapsid might be a naked core or be surrounded by a membranous envelope.
- COVALENTLY CLOSED CIRCULAR DNA
-
(cccDNA). The double-stranded cccDNA of HBV is the transcriptional template of HBV in the nucleus of infected cells.
- INTERNAL RIBOSOMAL ENTRY SITE
-
(IRES). A well-defined and highly conserved secondary structure located in the 5′ untranslated region of some viral and cellular mRNAs. It mediates the translation initiation of the viral message by a 5′-cap-independent mechanism.
- HBV e ANTIGEN
-
(Hepatitis B virus e antigen, HBeAg). HBeAg is derived from the pre-core polypeptide, which together with the core polypeptide, is encoded by the nucleocapsid open reading frame. After removal of the amino-terminal 29 amino acids of the pre-core polypeptide in the endoplasmic reticulum and trimming of the carboxyl terminus, the remaining polypeptide is secreted from infected cells as HBeAg. Neither pre-core polypeptide nor secreted HBeAg are required for HBV replication.
- ALANINE AMINOTRANSFERASE
-
(ALT). ALT is an intracellular enzyme that transfers amino groups from L-alanine to 2-ketoglutarate or from L-glutamic acid to pyruvate. It is released into the bloodstream when hepatocytes are damaged or die. The serum ALT level (upper limit of normal is 25–40 international units per litre, depending on the laboratory) is therefore an indicator of hepatocyte injury in acute and chronic hepatitis.
- EUKARYOTIC TRANSLATION INITIATION FACTOR 2α
-
(EIF2α). A mediator of translation initiation. Phosphorylation of EIF2α by the interferon-inducible double-stranded RNA-dependent protein kinase inhibits translation and thereby indirectly inhibits viral replication.
- COMPOUND GENOTYPE
-
A combination of two or more genotypes at loci encoding functionally related molecules.
- STEM LOOP
-
A hairpin structure that is formed by a single-stranded nucleic acid molecule when the ends of the molecule form a double helix (stem) based on complementary sequences and the central region remains single stranded and therefore forms a loop.
- EFFECTOR MEMORY CELL PHENOTYPE
-
Phenotype of terminally differentiated T cells. These cells lack lymph-node homing receptors but express receptors that enable them to home to inflamed tissues. Effector memory cells contain perforin and can exert immediate effector functions without the need for further differentiation.
- QUASISPECIES
-
A distribution of non-identical but closely related viral genomes. The entire distribution forms an organized cooperative structure, which functions as (quasi) a single unit (species).
- THALASSAEMIC
-
An individual suffering from thalassaemia, an inherited disorder of haemoglobin metabolism that results in reduced or absent production of one or more globin chains.
Rights and permissions
About this article
Cite this article
Rehermann, B., Nascimbeni, M. Immunology of hepatitis B virus and hepatitis C virus infection. Nat Rev Immunol 5, 215–229 (2005). https://doi.org/10.1038/nri1573
Issue Date:
DOI: https://doi.org/10.1038/nri1573
This article is cited by
-
Chronic LCMV infection regulates the effector T cell response by inducing the generation of less immunogenic dendritic cells
Experimental & Molecular Medicine (2023)
-
Extrahepatic Manifestations of Hepatitis B
Current Hepatology Reports (2023)
-
Hepatitis B virus promotes hepatocellular carcinoma development by activating GP73 to repress the innate immune response
Infectious Agents and Cancer (2022)
-
Anti-HBc IgG Levels: A Predictor of HBsAg Seroclearance in Chronic Hepatitis B Patients with Nucleos(t)ide Analogue-Induced HBeAg Seroclearance
Digestive Diseases and Sciences (2022)
-
An in silico study to unveil potential drugs and vaccine chimera for HBV capsid assembly protein: combined molecular docking and dynamics simulation approach
Journal of Molecular Modeling (2022)