Abstract
Mutations in the genes encoding pyrin and mevalonate kinase (MVK) cause distinct interleukin-1β (IL-1β)-mediated autoinflammatory diseases: familial Mediterranean fever (FMF) and hyperimmunoglobulinemia D syndrome (HIDS). Pyrin forms an inflammasome when mutant or in response to bacterial modification of the GTPase RhoA. We found that RhoA activated the serine-threonine kinases PKN1 and PKN2 that bind and phosphorylate pyrin. Phosphorylated pyrin bound to 14-3-3 proteins, regulatory proteins that in turn blocked the pyrin inflammasome. The binding of 14-3-3 and PKN proteins to FMF-associated mutant pyrin was substantially decreased, and the constitutive IL-1β release from peripheral blood mononuclear cells of patients with FMF or HIDS was attenuated by activation of PKN1 and PKN2. Defects in prenylation, seen in HIDS, led to RhoA inactivation and consequent pyrin inflammasome activation. These data suggest a previously unsuspected fundamental molecular connection between two seemingly distinct autoinflammatory disorders.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
References
Kastner, D.L., Aksentijevich, I. & Goldbach-Mansky, R. Autoinflammatory disease reloaded: a clinical perspective. Cell 140, 784–790 (2010).
Masters, S.L., Simon, A., Aksentijevich, I. & Kastner, D.L. Horror autoinflammaticus: the molecular pathophysiology of autoinflammatory disease. Annu. Rev. Immunol. 27, 621–668 (2009).
The International FMF Consortium. Ancient missense mutations in a new member of the RoRet gene family are likely to cause familial Mediterranean fever. Cell 90, 797–807 (1997).
Drenth, J.P. et al. Mutations in the gene encoding mevalonate kinase cause hyper-IgD and periodic fever syndrome. Nat. Genet. 22, 178–181 (1999).
Chae, J.J. et al. Gain-of-function Pyrin mutations induce NLRP3 protein-independent interleukin-1β activation and severe autoinflammation in mice. Immunity 34, 755–768 (2011).
Xu, H. et al. Innate immune sensing of bacterial modifications of Rho GTPases by the Pyrin inflammasome. Nature 513, 237–241 (2014).
Miziorko, H.M. Enzymes of the mevalonate pathway of isoprenoid biosynthesis. Arch. Biochem. Biophys. 505, 131–143 (2011).
Sohar, E., Gafni, J., Pras, M. & Heller, H. Familial Mediterranean fever. A survey of 470 cases and review of the literature. Am. J. Med. 43, 227–253 (1967).
French FMF Consortium. A candidate gene for familial Mediterranean fever. Nat. Genet. 17, 25–31 (1997).
Lachmann, H.J. et al. Clinical and subclinical inflammation in patients with familial Mediterranean fever and in heterozygous carriers of MEFV mutations. Rheumatology 45, 746–750 (2006).
Booty, M.G. et al. Familial Mediterranean fever with a single MEFV mutation: where is the second hit? Arthritis Rheum. 60, 1851–1861 (2009).
Marek-Yagel, D. et al. Clinical disease among patients heterozygous for familial Mediterranean fever. Arthritis Rheum. 60, 1862–1866 (2009).
Ozen, S. Changing concepts in familial Mediterranean fever: is it possible to have an autosomal-recessive disease with only one mutation? Arthritis Rheum. 60, 1575–1577 (2009).
Booth, D.R. et al. The genetic basis of autosomal dominant familial Mediterranean fever. Q. J. Med. 93, 217–221 (2000).
Aldea, A. et al. A severe autosomal-dominant periodic inflammatory disorder with renal AA amyloidosis and colchicine resistance associated to the MEFV H478Y variant in a Spanish kindred: an unusual familial Mediterranean fever phenotype or another MEFV-associated periodic inflammatory disorder? Am. J. Med. Genet. 124A, 67–73 (2004).
Jones, J.D. & Dangl, J.L. The plant immune system. Nature 444, 323–329 (2006).
Mackey, D., Holt, B.F. III, Wiig, A. & Dangl, J.L. RIN4 interacts with Pseudomonas syringae type III effector molecules and is required for RPM1-mediated resistance in Arabidopsis. Cell 108, 743–754 (2002).
Chae, J.J. et al. Targeted disruption of pyrin, the FMF protein, causes heightened sensitivity to endotoxin and a defect in macrophage apoptosis. Mol. Cell 11, 591–604 (2003).
Schoenwaelder, S.M. & Burridge, K. Evidence for a calpeptin-sensitive protein-tyrosine phosphatase upstream of the small GTPase Rho: a novel role for the calpain inhibitor calpeptin in the inhibition of protein-tyrosine phosphatases. J. Biol. Chem. 274, 14359–14367 (1999).
Schmidt, G. et al. Gln 63 of Rho is deamidated by Escherichia coli cytotoxic necrotizing factor-1. Nature 387, 725–729 (1997).
Flatau, G. et al. Toxin-induced activation of the G protein p21 Rho by deamidation of glutamine. Nature 387, 729–733 (1997).
Lee, G.S. et al. The calcium-sensing receptor regulates the NLRP3 inflammasome through Ca2+ and cAMP. Nature 492, 123–127 (2012).
Lang, P. et al. Protein kinase A phosphorylation of RhoA mediates the morphological and functional effects of cyclic AMP in cytotoxic lymphocytes. EMBO J. 15, 510–519 (1996).
Aburima, A. et al. cAMP signaling regulates platelet myosin light chain (MLC) phosphorylation and shape change through targeting the RhoA-Rho kinase-MLC phosphatase signaling pathway. Blood 122, 3533–3545 (2013).
Krendel, M., Zenke, F.T. & Bokoch, G.M. Nucleotide exchange factor GEF-H1 mediates cross-talk between microtubules and the actin cytoskeleton. Nat. Cell Biol. 4, 294–301 (2002).
Misawa, T. et al. Microtubule-driven spatial arrangement of mitochondria promotes activation of the NLRP3 inflammasome. Nat. Immunol. 14, 454–460 (2013).
Allam, R. et al. Mitochondrial apoptosis is dispensable for NLRP3 inflammasome activation but non-apoptotic caspase-8 is required for inflammasome priming. EMBO Rep. 15, 982–990 (2014).
Falk, M.D. et al. Enzyme kinetics and distinct modulation of the protein kinase N Family of kinases by lipid activators and small molecule inhibitors. Biosci. Rep. 34, e00097 (2014).
Feng, J. et al. Rho-associated kinase of chicken gizzard smooth muscle. J. Biol. Chem. 274, 3744–3752 (1999).
Yoshinaga, C., Mukai, H., Toshimori, M., Miyamoto, M. & Ono, Y. Mutational analysis of the regulatory mechanism of PKN: the regulatory region of PKN contains an arachidonic acid-sensitive autoinhibitory domain. J. Biochem. 126, 475–484 (1999).
Regan, J.W. EP2 and EP4 prostanoid receptor signaling. Life Sci. 74, 143–153 (2003).
Sokolowska, M. et al. Prostaglandin E2 inhibits NLRP3 inflammasome activation through EP4 receptor and intracellular cyclic AMP in human macrophages. J. Immunol. 194, 5472–5487 (2015).
Jéru, I. et al. Interaction of pyrin with 14.3.3 in an isoform-specific and phosphorylation-dependent manner regulates its translocation to the nucleus. Arthritis Rheum. 52, 1848–1857 (2005).
Mandey, S.H., Kuijk, L.M., Frenkel, J. & Waterham, H.R. A role for geranylgeranylation in interleukin-1beta secretion. Arthritis Rheum. 54, 3690–3695 (2006).
Kuijk, L.M. et al. HMG-CoA reductase inhibition induces IL-1beta release through Rac1/PI3K/PKB-dependent caspase-1 activation. Blood 112, 3563–3573 (2008).
Normand, S. et al. Specific increase in caspase-1 activity and secretion of IL-1 family cytokines: a putative link between mevalonate kinase deficiency and inflammation. Eur. Cytokine Netw. 20, 101–107 (2009).
Masters, S.L. et al. Familial autoinflammation with neutrophilic dermatosis reveals a regulatory mechanism of pyrin activation. Sci. Transl. Med. 8, 332ra45 (2016).
Vance, R.E. Immunology taught by bacteria. J. Clin. Immunol. 30, 507–511 (2010).
Ahuja, N., Kumar, P. & Bhatnagar, R. The adenylate cyclase toxins. Crit. Rev. Microbiol. 30, 187–196 (2004).
Chae, J.J. et al. The B30.2 domain of pyrin, the familial Mediterranean fever protein, interacts directly with caspase-1 to modulate IL-1beta production. Proc. Natl. Acad. Sci. USA 103, 9982–9987 (2006).
Acknowledgements
We thank the patients enrolled in our clinical protocols for providing research specimens, B. Barham, A. Jones, T. Romeo, P. Hoffmann, D. Stone, P. Pinto-Patarroyo, A. Ombrello and K. Barron for help with caring for patients, I. Aksentijevich for assistance in genotyping patients and for discussions, V. Dixit (Genentech) for ASC-, NLRP3- and NLRC4-deficient mice, R. Flavell (Yale University) for caspase-1-deficient mice, E. Alnemri (Thomas Jefferson University) for AIM2-deficient mice, and S. Masters and F. Shao for sharing data before publication. This work was supported by the Intramural Research Program of the National Human Genome Research Institute.
Author information
Authors and Affiliations
Contributions
Y.H.P., D.L.K. and J.J.C. designed the study. Y.H.P., G.W. and J.J.C. performed experiments. Y.H.P., G.W., D.L.K. and J.J.C. analyzed the data. Y.H.P., D.L.K. and J.J.C. wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 The pyrin inflammasome is activated by inactivation of RhoA.
(a) BMDMs from WT, Casp1, Asc, Nlrp3, Nlrc4, Aim2, Mefv-deficient mice, or C-terminal pyrin-truncation mice (Mefv∆Ct/∆Ct) were treated with LPS (1 µg/ml) and C3 toxin (0.5 µg/ml) for 6h. (b,c) BMDMs from WT mice were treated with LPS, C3 toxin, and the indicated concentration of (b) CNF toxin or (c) calpeptin for 6h. Cell culture supernatants were analyzed by IL-1β ELISA. ** P ≤ 0.005 and *** P ≤ 0.0005 (unpaired two-tailed t-test). Data represent the mean ± s.e.m from six independent experiments. (d,e) BMDMs from (d) WT mice were treated with LPS, C3 toxin, and calpeptin, or (e) MefvV726A/V726A mice were co-treated with LPS and calpeptin for 6h and then analyzed for IL-1β release by immunoblotting. (f) BMDMs from WT mice were co-treated with LPS, the indicated concentration of calpeptin for 5h, and then ATP for 0.5h, flagellin for 1h, or dsDNA for 1h. Cell culture supernatants (Sup) and cell lysates (Lys) were analyzed by immunoblotting as indicated. All immunoblot data shown are representative of at least three independent experiments.
Supplementary Figure 2 cAMP suppresses NLRP3 inflammasome activation but potentiates pyrin inflammasome activation.
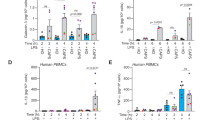
(a) PBMCs from FMF patients (designated patient number 1 and 2) with the indicated mutations in MEFV were non-primed or primed with LPS for 3h and then treated with the indicated dose of NKH477, a potent adenylate cyclase activator, for 1h. (b) PBMCs from CAPS patients (designated patient number 1 and 2) with the indicated mutations in NLRP3 were non-primed or primed with LPS (1 µg/ml) for 3h and then treated with the indicated concentration of NKH477 for 1h. (c) BMDMs from WT mice were primed with LPS (1 µg/ml) for 3h and then treated with ATP (2 mM) and the indicated concentration of NKH477 for 0.5h. Cell culture supernatants and cell lysates were analyzed by immunoblotting as indicated. All immunoblot data shown are representative of at least three independent experiments.
Supplementary Figure 3 RhoA effector kinases suppress pyrin inflammasome activation.
(a) LPS-primed BMDMs from WT or Mefv−/− mice were treated with the indicated dose of staurosporine or staurosporine (2 μM) and ATP (2 mM). (b,d) BMDMs from WT mice were co-treated with LPS and the indicated concentration of (b) bryostatin 1 or (d) arachidonic acid (AA) with C3 toxin for 6h. Cell culture supernatants were analyzed by IL-1β ELISA. ** P ≤ 0.005 (unpaired two-tailed t-test). Data represent the mean ± s.e.m from six independent experiments. (c,e) LPS-primed BMDMs from WT mice were treated with the indicated concentration of (c) bryostatin 1 or (e) arachidonic acid and ATP (2 mM) for 0.5h, dsDNA (1 µg/ml with 2.5 µl/ml of Lipofectamine 2000) for 1h, or flagellin (0.5 µg/ml with 25 µl/ml DOTAP) for 1h. Cell culture supernatants and cell lysates were analyzed by immunoblotting as indicated. All immunoblot data shown are representative of at least three independent experiments.
Supplementary Figure 4 Knock-in mice with the wild-type B30.2 domain of human pyrin have a milder inflammatory phenotype than that of knock-in mice with FMF-associated mutations.
(a) Lymphadenopathy and splenomegaly of FMF KI mice. The photograph shows lymph nodes and spleens from each of two 16 week-old Mefv+/+, MefvB30.2/B30.2, and MefvV726A/V726A mice. (b) Peripheral blood cells from Mefv+/+, MefvB30.2/B30.2, MefvM680I/M680I, MefvM694V/M694V, and MefvV726A/V726A mice were analyzed for CD11b+ myeloid cells. Numbers indicate percentage of total cells in gates. Each graph point represents one mouse, and means are shown as horizontal bars. * P ≤ 0.05 and *** P ≤ 0.0005 (unpaired two-tailed t-test).
Supplementary Figure 5 14-3-3 proteins bind to pyrin.
(a) The lysates of 239T cells transiently expressing full length or various deleted forms of pyrin (top) were immunoprecipitated with anti-myc antibody and analyzed by immunoblot for 14-3-3 proteins (bottom). (b) The lysates of 239T cells transiently expressing myc-tagged WT or the indicated mutant pyrin proteins were immunoprecipitated with anti-myc antibody and analyzed by immunoblot for 14-3-3 proteins. (c) The lysates of PT67 cells transiently expressing WT mouse pyrin or the indicated human B30.2 domain-fused mouse pyrin were immunoprecipitated with anti-myc antibody and analyzed by immunoblot for 14-3-3 proteins. (d) BMDMs from MefvV726A/V726A mice were co-treated with LPS and arachidonic acid or bryostatin 1. Cell lysates were immunoprecipitated with anti-pyrin antibody, and immune complexes were analyzed by immunoblot for 14-3-3ɛ and pyrin. (e) BMDMs from MefvV726A/V726A mice were co-treated with LPS and the indicated concentration of colchicine. Cell lysates were immunoprecipitated with anti-pyrin antibody, and immune complexes were analyzed by immunoblot for PKN1, 14-3-3ɛ, and pyrin. All immunoblot data shown are representative of at least three independent experiments.
Supplementary Figure 6 Proposed molecular mechanism of pyrin inflammasome activation.
Inactivation of RhoA by bacterial toxin-mediated modification, cAMP-mediated phosphorylation, or a defect of geranylgeranylation that causes HIDS leads to inactivation of the RhoA effector kinases, PKN1 and PKN2. Inactivation of effector kinases results in dephosphorylation of pyrin by yet unknown phosphatases and 14-3-3 protein dissociation. Free pyrin activates caspase-1 through the formation of a pyrin inflammasome.
Supplementary Figure 7 Proposed molecular mechanism of pyrin inflammasome activation caused by FMF-associated mutant pyrin.
FMF-associated mutant B30.2 domain inhibits the binding of RhoA effector kinases onto pyrin, which results in decreased phosphorylation of pyrin, decreased 14-3-3 binding to pyrin, and the activation of the pyrin inflammasome. The pyrin inflammasome can be suppressed by RhoA effector kinase activators, such as colchicine or arachidonic acid.
Supplementary Figure 8 HIDS is caused by the constitutive activation of the pyrin inflammasome.
(a) BMDMs from WT mice were treated with simvastatin (10 μM) for 16h and primed with LPS for 6h. Cell lysates were fractionated into membrane and cytosolic fractions, and analyzed by immunoblotting for RhoA. (b-d) BMDMs from WT, Nlrp3−/−, or Mefv−/− mice were treated with the indicated concentration of (b) simvastatin, (c) fluvastatin, or (d) lovastatin for 16h and primed with LPS for 6h. Cell culture supernatants and cell lysates were analyzed by immunoblotting as indicated. (e-g) BMDMs from WT mice were treated with simvastatin for 16h and co-treated with LPS and the indicated concentration of (e) geranylgeranyl pyrophosphate (GGpp), (f) arachidonic acid, or (g) bryostatin 1 for 6h. Cell culture supernatants were analyzed by IL-1β ELISA. ** P ≤ 0.005 (unpaired two-tailed t-test). Data represent the mean ± s.e.m from six independent experiments. (h) PBMCs from HIDS patients (designated patient number 3 and 4) with the indicated mutations in MVK were co-treated with LPS and the indicated concentration of colchicine for 6h. Cell culture supernatants and cell lysates were analyzed by immonoblotting as indicated. Immunoblot data shown are representative of one experiment (h) or at least three independent experiments (a-d, h).
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–8 (PDF 1379 kb)
Rights and permissions
About this article
Cite this article
Park, Y., Wood, G., Kastner, D. et al. Pyrin inflammasome activation and RhoA signaling in the autoinflammatory diseases FMF and HIDS. Nat Immunol 17, 914–921 (2016). https://doi.org/10.1038/ni.3457
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.3457